韓国で在宅高齢者のサルコペニアの有病割合をみた論文を紹介します。
Kim YS, Lee Y, Chung YS, Lee DJ, Joo NS, Hong D, Song GE, Kim HJ, Choi YJ, Kim KM: Prevalence of Sarcopenia and Sarcopenic Obesity in the Korean Population Based on the Fourth Korean National Health and Nutritional Examination Surveys. J Gerontol A Biol Sci Med Sci. 2012 Mar 19. [Epub ahead of print]
韓国で行っている健康栄養調査という大規模な調査データを用いてデータ分析しています。サルコペニアの診断基準は筋肉量のみで行っており、筋肉量減少が若年の1-2SD以下の場合クラスⅠ、2SD以下の場合クラスⅡとしています。骨格筋量を身長で補正したものと体重で補正したもので検討しています。
結果ですが以下、身長で補正した場合のみ示します。クラスⅡサルコペニアのカットオフ値は男性6.58kg/m2、女性4.59kg/m2です。クラスⅡサルコペニアと判定されたのは男性12.4%、女性0.1%でした。サルコペニア肥満は男女ともほとんど0でした。肥満は腹囲が男性90cm以上、女性85cm以上で判定しています。
以上より、身長で補正したサルコペニアの定義では、サルコペニアとサルコペニア肥満の有病割合を低く見積もる傾向があるという結論です。サルコペニア肥満は韓国の在宅高齢者にはほとんど存在しないということになりますね。
ただこれはカットオフ値が低すぎることが原因だと思います。真田らの日本人でのサルコペニア研究のカットオフ値は、男性6.87kg/m2、女性5.46kg/m2です。男性は大差ありませんが、女性はかなり異なります。なお、真田らのデータでも私はカットオフ値が低すぎで、改善の余地があるのではと私は感じています。
Abstract
BACKGROUND:
Sarcopenia is an important factor of functional impairment related to aging. This study is conducted to investigate the prevalence of sarcopenia and sarcopenic obesity in Korean population.
METHODS:
Representative Korean men (4,486) and women (5,999) aged 20 years or older were analyzed from the Fourth Korean National Health and Nutritional Examination Surveys. Sarcopenia was classified into Class I defined relative skeletal muscle mass loss within 1-2 SD of the gender-specific mean for healthy young adults and Class II below 2 SD. Relative skeletal muscle mass was represented by the appendicular skeletal muscle mass adjusted by height and body weight. Sarcopenic obesity was considered present in Class II sarcopenic participants whose waist circumference was more than or equal to 90 cm for men and more than or equal to 85 cm for women, respectively.
RESULTS:
The prevalence of Class II sarcopenia in the Korean elderly population was 12.4% for men and 0.1% for women by height-adjusted definition and 9.7% for men and 11.8% for women by weight-adjusted definition. The prevalence of sarcopenic obesity was 7.6% for men and 9.1% for women by weight-adjusted definition but nearly zero for men and women by height-adjusted definition. The prevalence of sarcopenia increased with age for men but for women only when applied with weight-adjusted definition.
CONCLUSIONS:
The prevalence of sarcopenia and sarcopenic obesity differs by gender and definition criteria. The height-adjusted definition may tend to underestimate the prevalence of sarcopenia and sarcopenic obesity, especially in women.
2012年3月29日木曜日
老人ホームでのサルコペニアの有病割合
老人ホームでのサルコペニアの有病割合とリスク因子を調査した論文を紹介します。
Landi F, Liperoti R, Fusco D, Mastropaolo S, Quattrociocchi D, Proia A, Russo A, Bernabei R, Onder G: Prevalence and risk factors of sarcopenia among nursing home older residents. J Gerontol A Biol Sci Med Sci. 2012 Jan;67(1):48-55.
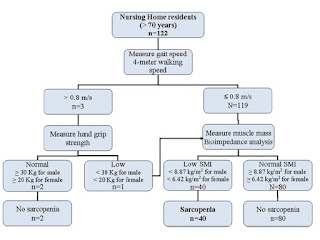
サルコペニアの診断基準は下記のように、European Working Group on Sarcopenia in Older People (EWGSOP)のものを用いています。筋肉量低下はBIA、筋力低下は握力、身体機能低下は4m歩行速度で評価しています。
結果ですが、老人ホーム入所中の70歳以上の高齢者のうち、32.8%がサルコペニアと判定されました。男性68%、女性21%と明らかな性差を認めました。その他のリスク因子として、脳血管疾患、変形性関節症、BMI21以下、余暇の身体活動が1日1時間以下を認めました。
なお、4m歩行速度の平均値は全体で0.14±0.20m/sですので、歩行不可の方が少なからず存在していることが推測されます。また、握力の平均値は全体で8.2±6.8kgで、0kgに近い方もいると思われます。BMIの平均値は全体で21.7±4.5、アルブミンは3.12±0.52g/dlでした。
イタリアの老人ホームで32.8%がサルコペニアであれば、日本の老人ホームでは大半がサルコペニアと判定されるのではないかと推測します。サルコペニアの診断基準ができてまだ日が浅いので、日本でもいろんな施設で有病割合をみる研究が行われるとよいと思います。
Abstract
BACKGROUND AND AIMS: Sarcopenia has been indicated as a reliable marker of frailty and poor prognosis among the oldest individuals. At present, there are no data on sarcopenia in nursing home population. We evaluated the prevalence of sarcopenia and its association with functional and clinical status in a population of elderly persons aged 70 years and older living in nursing homes.
METHODS: This study was conducted selecting all the participants (n = 122) living in the teaching nursing homes of Catholic University of Rome who were aged 70 years and older from August 1, 2010, to September 30, 2010. The European Working Group on Sarcopenia in Older People (EWGSOP) criteria were adopted. Accordingly, diagnosis of sarcopenia required the documentation of low muscle mass plus the documentation of either low muscle strength or low physical performance.
RESULTS: Forty residents (32.8%) were identified as affected by sarcopenia. The multivariate logistic regression analysis showed a high increase in risk of sarcopenia for male residents (odds ratio [OR] 13.39; 95% confidence interval [CI] 3.51-50.63) and for residents affected by cerebrovascular disease (OR 5.16; 95% CI 1.03-25.87) or osteoarthritis (OR 7.24; 95% CI 2.02-25.95). Residents who had a body mass index higher than 21 kg/m(2) had a lower risk to be sarcopenic (OR 0.76; 95% CI 0.64-0.90) relative to those with body mass index less than 21 kg/m(2). Similarly, sarcopenia was less likely to be present among participants involved in leisure physical activity for 1 hour or more per day (OR 0.40; 95% CI 0.12-0.98).
CONCLUSIONS: The present study suggests that among participants living in nursing homes, sarcopenia is highly prevalent and it is more represented among male residents (68%) than among female residents (21%). Our findings support the hypothesis that muscle mass is strongly associated with nutritional status and physical activity in nursing homes, too.
Landi F, Liperoti R, Fusco D, Mastropaolo S, Quattrociocchi D, Proia A, Russo A, Bernabei R, Onder G: Prevalence and risk factors of sarcopenia among nursing home older residents. J Gerontol A Biol Sci Med Sci. 2012 Jan;67(1):48-55.
サルコペニアの診断基準は下記のように、European Working Group on Sarcopenia in Older People (EWGSOP)のものを用いています。筋肉量低下はBIA、筋力低下は握力、身体機能低下は4m歩行速度で評価しています。
結果ですが、老人ホーム入所中の70歳以上の高齢者のうち、32.8%がサルコペニアと判定されました。男性68%、女性21%と明らかな性差を認めました。その他のリスク因子として、脳血管疾患、変形性関節症、BMI21以下、余暇の身体活動が1日1時間以下を認めました。
なお、4m歩行速度の平均値は全体で0.14±0.20m/sですので、歩行不可の方が少なからず存在していることが推測されます。また、握力の平均値は全体で8.2±6.8kgで、0kgに近い方もいると思われます。BMIの平均値は全体で21.7±4.5、アルブミンは3.12±0.52g/dlでした。
イタリアの老人ホームで32.8%がサルコペニアであれば、日本の老人ホームでは大半がサルコペニアと判定されるのではないかと推測します。サルコペニアの診断基準ができてまだ日が浅いので、日本でもいろんな施設で有病割合をみる研究が行われるとよいと思います。
Abstract
BACKGROUND AND AIMS: Sarcopenia has been indicated as a reliable marker of frailty and poor prognosis among the oldest individuals. At present, there are no data on sarcopenia in nursing home population. We evaluated the prevalence of sarcopenia and its association with functional and clinical status in a population of elderly persons aged 70 years and older living in nursing homes.
METHODS: This study was conducted selecting all the participants (n = 122) living in the teaching nursing homes of Catholic University of Rome who were aged 70 years and older from August 1, 2010, to September 30, 2010. The European Working Group on Sarcopenia in Older People (EWGSOP) criteria were adopted. Accordingly, diagnosis of sarcopenia required the documentation of low muscle mass plus the documentation of either low muscle strength or low physical performance.
RESULTS: Forty residents (32.8%) were identified as affected by sarcopenia. The multivariate logistic regression analysis showed a high increase in risk of sarcopenia for male residents (odds ratio [OR] 13.39; 95% confidence interval [CI] 3.51-50.63) and for residents affected by cerebrovascular disease (OR 5.16; 95% CI 1.03-25.87) or osteoarthritis (OR 7.24; 95% CI 2.02-25.95). Residents who had a body mass index higher than 21 kg/m(2) had a lower risk to be sarcopenic (OR 0.76; 95% CI 0.64-0.90) relative to those with body mass index less than 21 kg/m(2). Similarly, sarcopenia was less likely to be present among participants involved in leisure physical activity for 1 hour or more per day (OR 0.40; 95% CI 0.12-0.98).
CONCLUSIONS: The present study suggests that among participants living in nursing homes, sarcopenia is highly prevalent and it is more represented among male residents (68%) than among female residents (21%). Our findings support the hypothesis that muscle mass is strongly associated with nutritional status and physical activity in nursing homes, too.
2012年3月28日水曜日
サルコペニアの起源の論文
Rosenbergによるサルコペニアの起源の論文を紹介します。
Irwin H. Rosenberg. Sarcopenia: Origins and Clinical Relevance. J. Nutr. May 1, 1997 vol. 127 no. 5 990S-991S
下記のHPで全文見ることができます。2頁と短いので、ぜひ英語が得意でない方も挑戦してください。
http://jn.nutrition.org/content/127/5/990S.full
移動、経口摂取、自立、呼吸に影響を与える、加齢による除脂肪体重の減少を意味することばが、以前はありませんでした。そのため、1988年のニューメキシコのミーティングで、Rosenbergによってサルコペニアということばが生まれました。
sarcomalaciaかsarcopeniaのいずれかにしようという話だったようです。サルコマラシア(筋肉軟化症)ではことばの響きもあまりよくないですし、サルコペニアでよかったと思います(笑)。
この論文では、筋肉量減少の原因として、加齢のみを考えています。また、筋肉量減少だけでなく筋肉量減少による機能低下を含んでいます。加齢以外の原因による二次性サルコペニアや筋力低下は考慮されていません。二次性サルコペニアよるミオペニアということばのほうがよいのかもしれませんね。
Abstract
This presentation reflects on the origins of the term sarcopenia. The Greek roots of the word are sarx for flesh and penia for loss. The term actually describes important changes in body composition and related functions. Clearly defining sarcopenia will allow investigators to appropriately classify patients and examine underlying pathogenic mechanisms and will allow funding agencies to appropriately target research funds to a taxonomically distinct syndrome.
補足ですが、サルコペニアということばが最初に論文として紹介されたのは、1989年の下記のRosenbergの論文です。下記HPで全文PDFで見ることができます。
http://www.ajcn.org/content/50/5/1231.full.pdf
Irwin H. Rosenberg. Sarcopenia: Origins and Clinical Relevance. J. Nutr. May 1, 1997 vol. 127 no. 5 990S-991S
下記のHPで全文見ることができます。2頁と短いので、ぜひ英語が得意でない方も挑戦してください。
http://jn.nutrition.org/content/127/5/990S.full
移動、経口摂取、自立、呼吸に影響を与える、加齢による除脂肪体重の減少を意味することばが、以前はありませんでした。そのため、1988年のニューメキシコのミーティングで、Rosenbergによってサルコペニアということばが生まれました。
sarcomalaciaかsarcopeniaのいずれかにしようという話だったようです。サルコマラシア(筋肉軟化症)ではことばの響きもあまりよくないですし、サルコペニアでよかったと思います(笑)。
この論文では、筋肉量減少の原因として、加齢のみを考えています。また、筋肉量減少だけでなく筋肉量減少による機能低下を含んでいます。加齢以外の原因による二次性サルコペニアや筋力低下は考慮されていません。二次性サルコペニアよるミオペニアということばのほうがよいのかもしれませんね。
Abstract
This presentation reflects on the origins of the term sarcopenia. The Greek roots of the word are sarx for flesh and penia for loss. The term actually describes important changes in body composition and related functions. Clearly defining sarcopenia will allow investigators to appropriately classify patients and examine underlying pathogenic mechanisms and will allow funding agencies to appropriately target research funds to a taxonomically distinct syndrome.
補足ですが、サルコペニアということばが最初に論文として紹介されたのは、1989年の下記のRosenbergの論文です。下記HPで全文PDFで見ることができます。
http://www.ajcn.org/content/50/5/1231.full.pdf
栄養良好な大腿骨頸部骨折の栄養介入
もう1つ同じグループの、栄養状態良好~軽度低栄養の大腿骨頸部骨折患者に対する栄養介入のランダム化比較試験を紹介します。
Botella-Carretero JI, Iglesias B, Balsa JA, Zamarrón I, Arrieta F, Vázquez C: Effects of oral nutritional supplements in normally nourished or mildly undernourished geriatric patients after surgery for hip fracture: a randomized clinical trial. JPEN J Parenter Enteral Nutr. 2008 Mar-Apr;32(2):120-8.
リサーチクエスチョンは、
P:大腿骨頸部骨折の高齢患者に
I:術後に経口栄養剤を投与すると(蛋白質36gのみの群と、蛋白質37.6g、エネルギー500kcalの群)
C:経口栄養剤を投与しない場合と比較して
O:退院時の血清アルブミン、プレアルブミン、レチノール結合蛋白が改善するか
D:マスキングのないRCT
です。
MNAの平均得点は対照群19.4、蛋白質群18.7、エネルギー群20.5です。結果ですが、白丸が対照群、黒丸ら蛋白群、黒四角がエネルギー群です。3群間で血清アルブミン、プレアルブミン、レチノール結合蛋白に統計学的有意差を認めませんでした。BMI、AC、TSFも同様に統計学的有意差を認めませんでした。
栄養状態良好~軽度低栄養の大腿骨頸部骨折患者に対する術後の栄養介入で、血清アルブミン、プレアルブミン、レチノール結合蛋白は明らかな改善を認めないという結論になります。やはり低栄養と判定される大腿骨頸部骨折患者に対して、栄養+運動介入をしたいところです。
Abstract
BACKGROUND: Oral nutritional supplements have been recommended after orthopedic surgery in geriatric patients to reduce postoperative complications. However, tolerability of supplements could be a limitation, and their universal use is not supported by the heterogeneity of previous studies, especially in patients without malnutrition.
METHODS: This study is a randomized, controlled, open, parallel, 3-arm clinical trial comparing supplementation with protein powder dissolved in liquids to aim at 36 g of protein per day, energy and protein supplements to aim at 37.6 g of protein and 500 kcal per day, or no intervention in normally nourished or mildly undernourished patients. Outcomes were serum albumin, prealbumin, retinol-binding globulin, and body mass index, among others. Postoperative complications were also recorded.
RESULTS: Ninety patients aged 83.8 +/- 6.6 years were included. The mean ingested amount of supplements was 41.1% +/- 20.6% in the protein powder supplement group and 51.4% +/- 13.2% in the energy protein supplement group (t = 2.278, P = .027). Postoperative supplements had no effect on the nutrition status during in-hospital follow-up, as assessed by serum albumin (P = .251), prealbumin (P = .530), retinol-binding globulin (P = .552), or body mass index (P = .582). Multivariate analysis showed that length of hospital stay with an established complication until its resolution (beta = .230, P = .031), total hospital stay (beta = .450, P < .001), baseline body mass index (beta = .204, P = .045), and total daily ingested proteins per body weight (beta = .252, P = .018) were predictive variables on the change in serum albumin (R2 = 0.409, F = 11.246, P < .001).
CONCLUSIONS: Oral nutritional supplements in normally nourished or only mildly undernourished geriatric patients with hip fracture submitted to surgery may be of interest for patients with postoperative complications and long hospital stays
Botella-Carretero JI, Iglesias B, Balsa JA, Zamarrón I, Arrieta F, Vázquez C: Effects of oral nutritional supplements in normally nourished or mildly undernourished geriatric patients after surgery for hip fracture: a randomized clinical trial. JPEN J Parenter Enteral Nutr. 2008 Mar-Apr;32(2):120-8.
リサーチクエスチョンは、
P:大腿骨頸部骨折の高齢患者に
I:術後に経口栄養剤を投与すると(蛋白質36gのみの群と、蛋白質37.6g、エネルギー500kcalの群)
C:経口栄養剤を投与しない場合と比較して
O:退院時の血清アルブミン、プレアルブミン、レチノール結合蛋白が改善するか
D:マスキングのないRCT
です。
MNAの平均得点は対照群19.4、蛋白質群18.7、エネルギー群20.5です。結果ですが、白丸が対照群、黒丸ら蛋白群、黒四角がエネルギー群です。3群間で血清アルブミン、プレアルブミン、レチノール結合蛋白に統計学的有意差を認めませんでした。BMI、AC、TSFも同様に統計学的有意差を認めませんでした。
栄養状態良好~軽度低栄養の大腿骨頸部骨折患者に対する術後の栄養介入で、血清アルブミン、プレアルブミン、レチノール結合蛋白は明らかな改善を認めないという結論になります。やはり低栄養と判定される大腿骨頸部骨折患者に対して、栄養+運動介入をしたいところです。
Abstract
BACKGROUND: Oral nutritional supplements have been recommended after orthopedic surgery in geriatric patients to reduce postoperative complications. However, tolerability of supplements could be a limitation, and their universal use is not supported by the heterogeneity of previous studies, especially in patients without malnutrition.
METHODS: This study is a randomized, controlled, open, parallel, 3-arm clinical trial comparing supplementation with protein powder dissolved in liquids to aim at 36 g of protein per day, energy and protein supplements to aim at 37.6 g of protein and 500 kcal per day, or no intervention in normally nourished or mildly undernourished patients. Outcomes were serum albumin, prealbumin, retinol-binding globulin, and body mass index, among others. Postoperative complications were also recorded.
RESULTS: Ninety patients aged 83.8 +/- 6.6 years were included. The mean ingested amount of supplements was 41.1% +/- 20.6% in the protein powder supplement group and 51.4% +/- 13.2% in the energy protein supplement group (t = 2.278, P = .027). Postoperative supplements had no effect on the nutrition status during in-hospital follow-up, as assessed by serum albumin (P = .251), prealbumin (P = .530), retinol-binding globulin (P = .552), or body mass index (P = .582). Multivariate analysis showed that length of hospital stay with an established complication until its resolution (beta = .230, P = .031), total hospital stay (beta = .450, P < .001), baseline body mass index (beta = .204, P = .045), and total daily ingested proteins per body weight (beta = .252, P = .018) were predictive variables on the change in serum albumin (R2 = 0.409, F = 11.246, P < .001).
CONCLUSIONS: Oral nutritional supplements in normally nourished or only mildly undernourished geriatric patients with hip fracture submitted to surgery may be of interest for patients with postoperative complications and long hospital stays
大腿骨頸部骨折の周術期経口栄養剤
正常~軽度低栄養の大腿骨頸部骨折に対する周術期の経口栄養剤投与の効果をみたランダム化比較試験を紹介します。
Botella-Carretero JI, Iglesias B, Balsa JA, Arrieta F, Zamarrón I, Vázquez C: Perioperative oral nutritional supplements in normally or mildly undernourished geriatric patients submitted to surgery for hip fracture: a randomized clinical trial. Clin Nutr. 2010 Oct;29(5):574-9.
リサーチクエスチョンは、
P:大腿骨頸部骨折患者に
I:術前に栄養剤(1日400kcal、蛋白40g)を投与すると
C:栄養剤を投与しなかった場合と比較して
O:血清アルブミン、プレアルブミン、レチノール結合蛋白が改善するか
D:マスキングのないランダム化比較試験
です。
アウトカムとしてBMI、上腕周囲長、上腕三頭筋皮下脂肪厚も評価していますが、これらは周術期合併症の影響による体重減少や多量輸液や他の因子の影響も受ける可能性があるので、有意な変化を認めないのではないかということで、二次アウトカムとなっています。
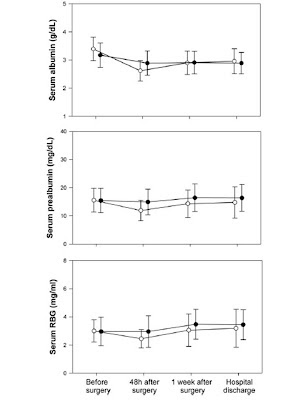
結果は下記の図のとおりです。栄養剤は実際には術前に6日間程度、平均52.2%摂取していました。
黒丸が介入群、白丸が対照群です。数値では示されていませんが、血清アルブミン、プレアルブミンは介入群で統計学的に有意に高値で推移しました。レチノール結合蛋白も統計学的有意差はありませんが、介入群で高値の傾向を示しました(p=0.089)。なおCRPの記載はありません。
二次アウトカムとしてBMI、AC、TSFは統計学的有意差を認めませんでした。入院期間、合併症(術後合併症に関してはp=0.091で介入群で少なめ)、退院先に関しても有意差を認めませんでした。ADLや歩行能力は、おそらく大差ないものと推測します。結論として周術期の経口栄養剤投与で血清蛋白がより早期に回復するとしています。
まず一次アウトカムを検査値のみとしていることが問題です。栄養状態(MNA、SGAなど)やADL、歩行能力の変化を一次アウトカムとすべきでしょう。今回はこれらの変化は明確にされていませんが、おそらく大きな変化は認めなかったものと思われます。ベースラインのMNAは対照群18.8点、介入群18.5点とAt riskです。
次に一次アウトカムに統計学的有意差は認めていますが、臨床的な有意差はあるでしょうか。図から推測する限り、介入群と対照群の差はアルブミンで0.3g/dl、プレアルブミンで3mg/dl程度に見えます。臨床的な意味がないとはもちろん言いませんが、臨床的に大きな差とはいえない気がします。
以上より正常~軽度低栄養の大腿骨頸部骨折に対する周術期の経口栄養剤投与の有効性は不十分だと思います。むしろ明らかに低栄養の大腿骨頸部骨折に対して、術前だけでなく術後も経口栄養剤を投与すべきではないでしょうか。
個人的にはこんなランダム化比較試験を回復期リハ病棟でできればと思うのですが、どなたかやってみませんか(笑)。
P:低栄養の大腿骨頸部骨折患者に
I:栄養剤(1日400kcal、蛋白20g、BCAA5g)を投与すると
C:栄養剤(1日200kcal、蛋白10g、BCAA2.5g)を投与する場合と比較して
O:ADLがより改善するか(二次アウトカムとして栄養状態、退院先がより改善するか)
D:一重マスキングのあるランダム化比較試験
Abstract
BACKGROUND: Oral nutritional supplements have been recommended after orthopedic surgery in geriatric patients. This has been shown to be effective even in normally nourished or mildly undernourished geriatric patients. Whether perioperative administration of these products is also effective and suitable is not known.
METHODS: Randomized, controlled, open, paralleled two-arms clinical trial, comparing energy-protein supplements (40 g of protein and 400 kcal per day), with no intervention in normally nourished or mildly undernourished patients. Outcomes were serum proteins, body mass index, postoperative complications among others.
RESULTS: 60 Elderly patients were included. Patients in the intervention group (n = 30) ingested 52.2 ± 12.1% of the prescribed supplements per day for 5.8 ± 1.8 days before surgery and until hospital discharge. There was a significant change in serum albumin at follow-up (F = 22.536, P < 0.001), and between the two groups (F = 5.763, P = 0.002), favouring the intervention. The same was observed for serum prealbumin (F = 6.654, P = 0.001 within subjects, F = 2.865, P = 0.045 for interaction). Logistic regression showed that only supplemented proteins per day (OR[95%CI] = 0.925[0.869-0.985]) were associated with less postoperative complications (R(2) = 0.323, χ(2) = 11.541, P = 0.003).
CONCLUSION: Perioperative supplements in geriatric patients with hip fracture submitted to surgery showed better recovery of plasma proteins. Higher daily protein intakes were associated with less postoperative complications.
Botella-Carretero JI, Iglesias B, Balsa JA, Arrieta F, Zamarrón I, Vázquez C: Perioperative oral nutritional supplements in normally or mildly undernourished geriatric patients submitted to surgery for hip fracture: a randomized clinical trial. Clin Nutr. 2010 Oct;29(5):574-9.
リサーチクエスチョンは、
P:大腿骨頸部骨折患者に
I:術前に栄養剤(1日400kcal、蛋白40g)を投与すると
C:栄養剤を投与しなかった場合と比較して
O:血清アルブミン、プレアルブミン、レチノール結合蛋白が改善するか
D:マスキングのないランダム化比較試験
です。
アウトカムとしてBMI、上腕周囲長、上腕三頭筋皮下脂肪厚も評価していますが、これらは周術期合併症の影響による体重減少や多量輸液や他の因子の影響も受ける可能性があるので、有意な変化を認めないのではないかということで、二次アウトカムとなっています。
結果は下記の図のとおりです。栄養剤は実際には術前に6日間程度、平均52.2%摂取していました。
黒丸が介入群、白丸が対照群です。数値では示されていませんが、血清アルブミン、プレアルブミンは介入群で統計学的に有意に高値で推移しました。レチノール結合蛋白も統計学的有意差はありませんが、介入群で高値の傾向を示しました(p=0.089)。なおCRPの記載はありません。
二次アウトカムとしてBMI、AC、TSFは統計学的有意差を認めませんでした。入院期間、合併症(術後合併症に関してはp=0.091で介入群で少なめ)、退院先に関しても有意差を認めませんでした。ADLや歩行能力は、おそらく大差ないものと推測します。結論として周術期の経口栄養剤投与で血清蛋白がより早期に回復するとしています。
まず一次アウトカムを検査値のみとしていることが問題です。栄養状態(MNA、SGAなど)やADL、歩行能力の変化を一次アウトカムとすべきでしょう。今回はこれらの変化は明確にされていませんが、おそらく大きな変化は認めなかったものと思われます。ベースラインのMNAは対照群18.8点、介入群18.5点とAt riskです。
次に一次アウトカムに統計学的有意差は認めていますが、臨床的な有意差はあるでしょうか。図から推測する限り、介入群と対照群の差はアルブミンで0.3g/dl、プレアルブミンで3mg/dl程度に見えます。臨床的な意味がないとはもちろん言いませんが、臨床的に大きな差とはいえない気がします。
以上より正常~軽度低栄養の大腿骨頸部骨折に対する周術期の経口栄養剤投与の有効性は不十分だと思います。むしろ明らかに低栄養の大腿骨頸部骨折に対して、術前だけでなく術後も経口栄養剤を投与すべきではないでしょうか。
個人的にはこんなランダム化比較試験を回復期リハ病棟でできればと思うのですが、どなたかやってみませんか(笑)。
P:低栄養の大腿骨頸部骨折患者に
I:栄養剤(1日400kcal、蛋白20g、BCAA5g)を投与すると
C:栄養剤(1日200kcal、蛋白10g、BCAA2.5g)を投与する場合と比較して
O:ADLがより改善するか(二次アウトカムとして栄養状態、退院先がより改善するか)
D:一重マスキングのあるランダム化比較試験
Abstract
BACKGROUND: Oral nutritional supplements have been recommended after orthopedic surgery in geriatric patients. This has been shown to be effective even in normally nourished or mildly undernourished geriatric patients. Whether perioperative administration of these products is also effective and suitable is not known.
METHODS: Randomized, controlled, open, paralleled two-arms clinical trial, comparing energy-protein supplements (40 g of protein and 400 kcal per day), with no intervention in normally nourished or mildly undernourished patients. Outcomes were serum proteins, body mass index, postoperative complications among others.
RESULTS: 60 Elderly patients were included. Patients in the intervention group (n = 30) ingested 52.2 ± 12.1% of the prescribed supplements per day for 5.8 ± 1.8 days before surgery and until hospital discharge. There was a significant change in serum albumin at follow-up (F = 22.536, P < 0.001), and between the two groups (F = 5.763, P = 0.002), favouring the intervention. The same was observed for serum prealbumin (F = 6.654, P = 0.001 within subjects, F = 2.865, P = 0.045 for interaction). Logistic regression showed that only supplemented proteins per day (OR[95%CI] = 0.925[0.869-0.985]) were associated with less postoperative complications (R(2) = 0.323, χ(2) = 11.541, P = 0.003).
CONCLUSION: Perioperative supplements in geriatric patients with hip fracture submitted to surgery showed better recovery of plasma proteins. Higher daily protein intakes were associated with less postoperative complications.
2012年3月27日火曜日
栄養とサルコペニアのレビュー
栄養とサルコペニアのレビュー論文(学会抄録)を紹介します。ここでは原発性サルコペニア(加齢によるサルコペニア)に対する栄養療法がレビューされています。
D. Joe Millward: Nutrition and sarcopenia: evidence for an interaction. Proceedings of the Nutrition Society, FirstView Article : pp 1-10. The Annual Meeting of BAPEN with the Nutrition Society, Harrogate International Centre, Harrogate.29–30 November 2011
サルコペニアは活動的でおそらくは栄養状態良好な高齢者に認めるため、単純に栄養が原因というわけではなく、栄養療法の明確なエビデンスはかなり限定されています。蛋白やアミノ酸投与の介入研究の多くは無効という結果です。魚油は筋蛋白合成の同化抵抗性を緩和するという報告が1つあります。
抗酸化物質に関するエビデンスは少ないです。野菜や果物の摂取は野菜や果物に含まれるカリウムによってアシドーシスによるサルコペニアを防ぐ可能性があります。ビタミンD欠乏はサルコペニアやダイナペニアと関連していますが、欠乏レベル以上にビタミンDを高める影響に関しては限定され賛否両論です。
以上よりサルコペニアに対する栄養療法は、全般的に健康なライフスタイルを保つための栄養アドバイス以上のエビデンスはないという結論です。十分に活動しエネルギーと栄養素を摂取し、特に果物と野菜と魚油を十分に摂取しましょうということです。
加齢によるサルコペニアで栄養療法単独の効果を出すのはなかなか難しいと思います。運動療法とセットで考えるべきでしょう。一方、二次性サルコペニアで特に低栄養を合併している場合には、栄養療法単独でも有効な可能性が十分にあります。実際には運動療法の併用が必要ですので、単独の効果を示すのは容易ではありませんが。
Abstract
Nutritional interventions that might influence sarcopenia, as indicated by literature reporting on sarcopenia per se as well as dynapenia and frailty, are reviewed in relation to potential physiological aetiological factors, i.e. inactivity, anabolic resistance, inflammation, acidosis and vitamin D deficiency. As sarcopenia occurs in physically active and presumably well-nourished populations, it is argued that a simple nutritional aetiology is unlikely and unequivocal evidence for any nutritional influence is extremely limited. Dietary protein is probably the most widely researched nutrient but only for frailty is there one study showing evidence of an aetiological influence and most intervention studies with protein or amino acids have proved ineffective with only a very few exceptions. Fish oil has been shown to attenuate anabolic resistance of muscle protein synthesis in one study. There is limited evidence for a protective influence of antioxidants and inducers of phase 2 proteins on sarcopenia, dynapenia and anabolic resistance in human and animal studies. Also fruit and vegetables may protect against acidosis-induced sarcopenia through their provision of dietary potassium. While severe vitamin D deficiency is associated with dynapenia and sarcopenia, the evidence for a beneficial influence of increasing vitamin D status above the severe deficiency level is limited and controversial, especially in men. On this basis there is insufficient evidence for any more specific nutritional advice than that contained in the general healthy lifestyle–healthy diet message: i.e. avoiding inactivity and low intakes of food energy and nutrients and maintain an active lifestyle with a diet providing a rich supply of fruit and vegetables and frequent oily fish.
D. Joe Millward: Nutrition and sarcopenia: evidence for an interaction. Proceedings of the Nutrition Society, FirstView Article : pp 1-10. The Annual Meeting of BAPEN with the Nutrition Society, Harrogate International Centre, Harrogate.29–30 November 2011
サルコペニアは活動的でおそらくは栄養状態良好な高齢者に認めるため、単純に栄養が原因というわけではなく、栄養療法の明確なエビデンスはかなり限定されています。蛋白やアミノ酸投与の介入研究の多くは無効という結果です。魚油は筋蛋白合成の同化抵抗性を緩和するという報告が1つあります。
抗酸化物質に関するエビデンスは少ないです。野菜や果物の摂取は野菜や果物に含まれるカリウムによってアシドーシスによるサルコペニアを防ぐ可能性があります。ビタミンD欠乏はサルコペニアやダイナペニアと関連していますが、欠乏レベル以上にビタミンDを高める影響に関しては限定され賛否両論です。
以上よりサルコペニアに対する栄養療法は、全般的に健康なライフスタイルを保つための栄養アドバイス以上のエビデンスはないという結論です。十分に活動しエネルギーと栄養素を摂取し、特に果物と野菜と魚油を十分に摂取しましょうということです。
加齢によるサルコペニアで栄養療法単独の効果を出すのはなかなか難しいと思います。運動療法とセットで考えるべきでしょう。一方、二次性サルコペニアで特に低栄養を合併している場合には、栄養療法単独でも有効な可能性が十分にあります。実際には運動療法の併用が必要ですので、単独の効果を示すのは容易ではありませんが。
Abstract
Nutritional interventions that might influence sarcopenia, as indicated by literature reporting on sarcopenia per se as well as dynapenia and frailty, are reviewed in relation to potential physiological aetiological factors, i.e. inactivity, anabolic resistance, inflammation, acidosis and vitamin D deficiency. As sarcopenia occurs in physically active and presumably well-nourished populations, it is argued that a simple nutritional aetiology is unlikely and unequivocal evidence for any nutritional influence is extremely limited. Dietary protein is probably the most widely researched nutrient but only for frailty is there one study showing evidence of an aetiological influence and most intervention studies with protein or amino acids have proved ineffective with only a very few exceptions. Fish oil has been shown to attenuate anabolic resistance of muscle protein synthesis in one study. There is limited evidence for a protective influence of antioxidants and inducers of phase 2 proteins on sarcopenia, dynapenia and anabolic resistance in human and animal studies. Also fruit and vegetables may protect against acidosis-induced sarcopenia through their provision of dietary potassium. While severe vitamin D deficiency is associated with dynapenia and sarcopenia, the evidence for a beneficial influence of increasing vitamin D status above the severe deficiency level is limited and controversial, especially in men. On this basis there is insufficient evidence for any more specific nutritional advice than that contained in the general healthy lifestyle–healthy diet message: i.e. avoiding inactivity and low intakes of food energy and nutrients and maintain an active lifestyle with a diet providing a rich supply of fruit and vegetables and frequent oily fish.
2012年3月26日月曜日
同等性・非劣性の解析
週刊医学界新聞 第2971号 2012年03月26日で、今日から使える医療統計学講座【Lesson11】同等性・非劣性の解析の記事が掲載されています。
http://www.igaku-shoin.co.jp/paperDetail.do?id=PA02971_04
統計学的検定で統計学的有意差を検証するには、 p<0.05が1つの目安になります。一方、統計学的に同等であることを検証するには、p>0.05は目安になりません。これはあくまで統計学的有意差を検証できなかっただけであり、これで両群が同等かどうかはまったくわかりません。
今回は、同等性・非劣性の解析についてわかりやすく紹介されています。上記HPより引用です。「同等性を示すためにP値を用いることは禁じられています。"十分なサンプル数"で正確に同等だというために,同等性の解析にはP値ではなく信頼区間を用いる必要があります。」とあります。
ただし、このためには十分なサンプル数を確保することが必要になります。それは臨床研究を実施するうえでなかなか大変となるため、同等性研究の代替案として非劣性試験が行われるようになっています。以下、少し長いですが引用です。
「"非劣性"とは,すでに有効な治療薬が存在し,新薬は副作用が少ないなど既存薬よりも利点があるといった場合,既存薬に対し有効性において優越性が証明できなくても,劣っていないことが証明できればそれでよし,といった研究に使われます。同等性を示すマージンが両側であるのに対し,非劣性試験では,新薬が既存薬より劣っていないかどうかのみに注目し,新薬が既存薬より優れているという優越性が成り立っても成り立たなくてもよいので,信頼区間の片側のみに注目します。」
非劣性試験では、以下の3つを見ることができます。
優越性:"違いがない"という値(この場合はゼロ)を含まない。
同等性:臨床的に意味のある差の下限と上限(両側)のマージンの中にすべて入る。
非劣性:信頼区間の片方が非劣性マージン(片側)より小さい。
「優越性を目的として始められた研究であるのに,優越性が出なかったからと言って,途中から解釈が非劣性に変わっている研究をよく目にしますが,それはタブーです。」とあります。このような学会発表をよく見かけるのは私だけでしょうか。統計的有意差なし≠同等性だけでも、肝に銘じておきたいですね。
http://www.igaku-shoin.co.jp/paperDetail.do?id=PA02971_04
統計学的検定で統計学的有意差を検証するには、 p<0.05が1つの目安になります。一方、統計学的に同等であることを検証するには、p>0.05は目安になりません。これはあくまで統計学的有意差を検証できなかっただけであり、これで両群が同等かどうかはまったくわかりません。
今回は、同等性・非劣性の解析についてわかりやすく紹介されています。上記HPより引用です。「同等性を示すためにP値を用いることは禁じられています。"十分なサンプル数"で正確に同等だというために,同等性の解析にはP値ではなく信頼区間を用いる必要があります。」とあります。
ただし、このためには十分なサンプル数を確保することが必要になります。それは臨床研究を実施するうえでなかなか大変となるため、同等性研究の代替案として非劣性試験が行われるようになっています。以下、少し長いですが引用です。
「"非劣性"とは,すでに有効な治療薬が存在し,新薬は副作用が少ないなど既存薬よりも利点があるといった場合,既存薬に対し有効性において優越性が証明できなくても,劣っていないことが証明できればそれでよし,といった研究に使われます。同等性を示すマージンが両側であるのに対し,非劣性試験では,新薬が既存薬より劣っていないかどうかのみに注目し,新薬が既存薬より優れているという優越性が成り立っても成り立たなくてもよいので,信頼区間の片側のみに注目します。」
非劣性試験では、以下の3つを見ることができます。
優越性:"違いがない"という値(この場合はゼロ)を含まない。
同等性:臨床的に意味のある差の下限と上限(両側)のマージンの中にすべて入る。
非劣性:信頼区間の片方が非劣性マージン(片側)より小さい。
「優越性を目的として始められた研究であるのに,優越性が出なかったからと言って,途中から解釈が非劣性に変わっている研究をよく目にしますが,それはタブーです。」とあります。このような学会発表をよく見かけるのは私だけでしょうか。統計的有意差なし≠同等性だけでも、肝に銘じておきたいですね。
2012年3月25日日曜日
骨格筋の神経栄養因子の役割
Facebookで宇野さんに教えていただいた論文を紹介します。骨格筋における神経栄養因子の役割のレビュー論文です。
Kunihiro Sakuma and Akihiko Yamaguchi: The Recent Understanding of the Neurotrophin's Role in Skeletal Muscle Adaptation. Journal of Biomedicine and BiotechnologyVolume 2011 (2011), Article ID 201696, 12 pages doi:10.1155/2011/201696
豊橋技術科学大学の佐久間邦弘先生の論文です。佐久間先生の最近の実績は、佐久間研究室のHPの最新情報で確認できます。ここに掲載されている論文も順番に読んでいきたいですね。
http://www.health.tut.ac.jp/sakuma/news.html
論文自体は下記のHPで全文見ることができます。
http://www.hindawi.com/journals/jbb/2011/201696/
神経栄養因子は運動ニューロンの生存や機能だけでなく、筋芽細胞や筋線維の発達と分化にも関与しています。運動など筋肉収縮はBNDF(脳由来神経栄養因子)のmRNAと蛋白を骨格筋で産生します。BNDFは糖代謝を強化したり、ミオカインとして脳疾患(アルツハイマー病やうつ病)を改善させたりする役割をもつ可能性があります。
神経筋疾患の成人では、神経栄養因子の発現の変化を認め、こういった疾患における神経栄養因子の役割も解明されはじめています。サルコペニアと神経栄養因子に関する記載も本文にあります。また、学習と記憶におけるBNDFの役割への関心も高まっています。
基礎医学の論文を読むのは相変わらず苦手ですが、少しずつ慣れなければと感じています。BNDFについては、以下の日本語論文もわかりやすいかと思います。
野藤 悠,諏訪雅貴,佐々木 悠,熊谷秋三:脳由来神経栄養因子(BDNF)の役割と運動の影響.健康科学 31、p49-59
https://qir.kyushu-u.ac.jp/dspace/bitstream/2324/13951/1/p049.pdf
Abstract
This paper summarizes the various effects of neurotrophins in skeletal muscle and how these proteins act as potential regulators of the maintenance, function, and regeneration of skeletal muscle fibers. Increasing evidence suggests that this family of neurotrophic factors influence not only the survival and function of innervating motoneurons but also the development and differentiation of myoblasts and muscle fibers. Muscle contractions (e.g., exercise) produce BDNF mRNA and protein in skeletal muscle, and the BDNF seems to play a role in enhancing glucose metabolism and may act for myokine to improve various brain disorders (e.g., Alzheimer's disease and major depression). In adults with neuromuscular disorders, variations in neurotrophin expression are found, and the role of neurotrophins under such conditions is beginning to be elucidated. This paper provides a basis for a better understanding of the role of these factors under such pathological conditions and for treatment of human neuromuscular disease.
Kunihiro Sakuma and Akihiko Yamaguchi: The Recent Understanding of the Neurotrophin's Role in Skeletal Muscle Adaptation. Journal of Biomedicine and BiotechnologyVolume 2011 (2011), Article ID 201696, 12 pages doi:10.1155/2011/201696
豊橋技術科学大学の佐久間邦弘先生の論文です。佐久間先生の最近の実績は、佐久間研究室のHPの最新情報で確認できます。ここに掲載されている論文も順番に読んでいきたいですね。
http://www.health.tut.ac.jp/sakuma/news.html
論文自体は下記のHPで全文見ることができます。
http://www.hindawi.com/journals/jbb/2011/201696/
神経栄養因子は運動ニューロンの生存や機能だけでなく、筋芽細胞や筋線維の発達と分化にも関与しています。運動など筋肉収縮はBNDF(脳由来神経栄養因子)のmRNAと蛋白を骨格筋で産生します。BNDFは糖代謝を強化したり、ミオカインとして脳疾患(アルツハイマー病やうつ病)を改善させたりする役割をもつ可能性があります。
神経筋疾患の成人では、神経栄養因子の発現の変化を認め、こういった疾患における神経栄養因子の役割も解明されはじめています。サルコペニアと神経栄養因子に関する記載も本文にあります。また、学習と記憶におけるBNDFの役割への関心も高まっています。
基礎医学の論文を読むのは相変わらず苦手ですが、少しずつ慣れなければと感じています。BNDFについては、以下の日本語論文もわかりやすいかと思います。
野藤 悠,諏訪雅貴,佐々木 悠,熊谷秋三:脳由来神経栄養因子(BDNF)の役割と運動の影響.健康科学 31、p49-59
https://qir.kyushu-u.ac.jp/dspace/bitstream/2324/13951/1/p049.pdf
Abstract
This paper summarizes the various effects of neurotrophins in skeletal muscle and how these proteins act as potential regulators of the maintenance, function, and regeneration of skeletal muscle fibers. Increasing evidence suggests that this family of neurotrophic factors influence not only the survival and function of innervating motoneurons but also the development and differentiation of myoblasts and muscle fibers. Muscle contractions (e.g., exercise) produce BDNF mRNA and protein in skeletal muscle, and the BDNF seems to play a role in enhancing glucose metabolism and may act for myokine to improve various brain disorders (e.g., Alzheimer's disease and major depression). In adults with neuromuscular disorders, variations in neurotrophin expression are found, and the role of neurotrophins under such conditions is beginning to be elucidated. This paper provides a basis for a better understanding of the role of these factors under such pathological conditions and for treatment of human neuromuscular disease.
2012年3月24日土曜日
横隔膜は加齢による変化を認めない
高齢ラットの横隔膜は加齢による変化を認めないという研究を紹介します。
Andreas N. Kavazis, Keith C. DeRuisseau and Donna M. Gordon: The senescent rat diaphragm does not exhibit age-related changes in caspase activities, DNA fragmentation, or myonuclear domain. European Journal of Applied Physiology DOI: 10.1007/s00421-012-2380-2 Online First
抄録しか読んでいませんが、若いラットと高齢ラットで、横隔膜のタンパク質カルボニル(フリーラジカルによるタンパク質酸化の指標)、カスパーゼ活性化(細胞にアポトーシスを起こさせるシグナル伝達経路を構成)、DNA断片化、筋線維断面積、筋核ドメインを比較しました。
その結果、いずれも若いラットと高齢ラットで有意差を認めませんでした。これより横隔膜は加齢による変化や筋萎縮を認めないという結論です。あくまでラットでの話ですので、ヒトでそのまま当てはまるかどうかはわかりません。
加齢によるサルコペニアは、横隔膜では認めないのかもしれません。しかし、活動(人工呼吸器装着による廃用)、栄養(飢餓)、疾患(侵襲、悪液質、神経筋疾患)による二次性サルコペニアは、横隔膜にも認めると推測します。リハ栄養では老年医学以上に呼吸筋のサルコペニアが重要かもしれません。
Abstract
The diaphragm muscle is essential for normal ventilation and it is chronically active throughout the lifespan. In most skeletal muscles, aging is associated with increased oxidative stress and myofiber atrophy. Since the diaphragm maintains a unique chronic contractile activity, we hypothesized that these alterations would not occur in senescent diaphragms compared to young diaphragms. In addition, we investigated whether senescence leads to altered diaphragmatic caspase activity and myonuclear domain. We harvested diaphragm muscles from 6 and 24–26 month old male Fisher 344 rats (n = 10 per group). Measurements of protein carbonyls, caspase 2, 3, 9, and 12 activities, DNA fragmentation, myofiber cross-sectional area, and myonuclear domain of diaphragm muscles were performed. No age-related changes (p > 0.05) in diaphragmatic protein oxidation or activities of caspase 2, 3, 9, and 12 were observed between groups. In addition, DNA fragmentation, as detected by the ligation-mediated polymerase chain reaction ladder assay, was not different (p > 0.05) between young and senescent diaphragms. Importantly, the cross-sectional area and myonuclear domain of diaphragm myofibers from senescent animals were also not different (p > 0.05) from young diaphragms. In conclusion, our data show that the senescent diaphragm does not atrophy or exhibit changes in select markers of the apoptotic pathway and this may be a result of the diaphragm’s unique continuous contractile activity.
Andreas N. Kavazis, Keith C. DeRuisseau and Donna M. Gordon: The senescent rat diaphragm does not exhibit age-related changes in caspase activities, DNA fragmentation, or myonuclear domain. European Journal of Applied Physiology DOI: 10.1007/s00421-012-2380-2 Online First
抄録しか読んでいませんが、若いラットと高齢ラットで、横隔膜のタンパク質カルボニル(フリーラジカルによるタンパク質酸化の指標)、カスパーゼ活性化(細胞にアポトーシスを起こさせるシグナル伝達経路を構成)、DNA断片化、筋線維断面積、筋核ドメインを比較しました。
その結果、いずれも若いラットと高齢ラットで有意差を認めませんでした。これより横隔膜は加齢による変化や筋萎縮を認めないという結論です。あくまでラットでの話ですので、ヒトでそのまま当てはまるかどうかはわかりません。
加齢によるサルコペニアは、横隔膜では認めないのかもしれません。しかし、活動(人工呼吸器装着による廃用)、栄養(飢餓)、疾患(侵襲、悪液質、神経筋疾患)による二次性サルコペニアは、横隔膜にも認めると推測します。リハ栄養では老年医学以上に呼吸筋のサルコペニアが重要かもしれません。
Abstract
The diaphragm muscle is essential for normal ventilation and it is chronically active throughout the lifespan. In most skeletal muscles, aging is associated with increased oxidative stress and myofiber atrophy. Since the diaphragm maintains a unique chronic contractile activity, we hypothesized that these alterations would not occur in senescent diaphragms compared to young diaphragms. In addition, we investigated whether senescence leads to altered diaphragmatic caspase activity and myonuclear domain. We harvested diaphragm muscles from 6 and 24–26 month old male Fisher 344 rats (n = 10 per group). Measurements of protein carbonyls, caspase 2, 3, 9, and 12 activities, DNA fragmentation, myofiber cross-sectional area, and myonuclear domain of diaphragm muscles were performed. No age-related changes (p > 0.05) in diaphragmatic protein oxidation or activities of caspase 2, 3, 9, and 12 were observed between groups. In addition, DNA fragmentation, as detected by the ligation-mediated polymerase chain reaction ladder assay, was not different (p > 0.05) between young and senescent diaphragms. Importantly, the cross-sectional area and myonuclear domain of diaphragm myofibers from senescent animals were also not different (p > 0.05) from young diaphragms. In conclusion, our data show that the senescent diaphragm does not atrophy or exhibit changes in select markers of the apoptotic pathway and this may be a result of the diaphragm’s unique continuous contractile activity.
サルコペニアの書籍
サルコペニアがタイトルに入っている書籍は、日本語では「サルコペニアの基礎と臨床」しか現時点ではありませんが、英語では何冊か出ています。
Gordon S. Lynch: Sarcopenia: Age-Related Muscle Wasting and Weakness: Mechanisms and Treatments. Springer (2010/12)
この書籍は以前に下記のブログで紹介しています。
http://rehabnutrition.blogspot.jp/2011/10/sarcopenia-age-related-muscle-wasting.html
Yves Rolland: Sarcopenia, An Issue of Clinics in Geriatric Medicine, 1e (The Clinics: Internal Medicine). Saunders (2011/8/29)
http://geriatric.theclinics.com/issues?issue_key=S0749-0690(11)X0003-4
書籍の概要(目次と抄録)だけでしたら、下記のHPでFreeで見ることができます。これを読むだけでもサルコペニアの学習になります。
http://download.journals.elsevierhealth.com/pdfs/journals/0749-0690/PIIS0749069011000577.pdf
Jordan R. Moon, Jeffrey R. Stout: Assessments of Fat-Free Mass and Sarcopenia in Older Adults. LAP Lambert Academic Publishing (2011/04)
こちらは80ページと薄いペーパーバッグですが、値段は安くありません。他のサルコペニアの書籍よりは見劣りするのではという気がします。
Alfonso J. Cruz-Jentoft, John E. Morley: Sarcopenia. Wiley (2012/10/2)
http://as.wiley.com/WileyCDA/WileyTitle/productCd-1119975875.html
この書籍は発行が9月なのでまだかなり先ですが、著者は間違いないですし360ページの書籍ですので、かなり期待できると思います。内容はまだわかりませんが…。
ただ、どの書籍も老年医学のサルコペニアに関する内容がほとんどです。研究が老年医学領域で進んでいるので当たり前ではありますが…。今後、リハ栄養のサルコペニア(広義:廃用・飢餓・疾患を含む)の書籍も作らなければと感じています。
Gordon S. Lynch: Sarcopenia: Age-Related Muscle Wasting and Weakness: Mechanisms and Treatments. Springer (2010/12)
この書籍は以前に下記のブログで紹介しています。
http://rehabnutrition.blogspot.jp/2011/10/sarcopenia-age-related-muscle-wasting.html
Yves Rolland: Sarcopenia, An Issue of Clinics in Geriatric Medicine, 1e (The Clinics: Internal Medicine). Saunders (2011/8/29)
http://geriatric.theclinics.com/issues?issue_key=S0749-0690(11)X0003-4
書籍の概要(目次と抄録)だけでしたら、下記のHPでFreeで見ることができます。これを読むだけでもサルコペニアの学習になります。
http://download.journals.elsevierhealth.com/pdfs/journals/0749-0690/PIIS0749069011000577.pdf
Jordan R. Moon, Jeffrey R. Stout: Assessments of Fat-Free Mass and Sarcopenia in Older Adults. LAP Lambert Academic Publishing (2011/04)
こちらは80ページと薄いペーパーバッグですが、値段は安くありません。他のサルコペニアの書籍よりは見劣りするのではという気がします。
Alfonso J. Cruz-Jentoft, John E. Morley: Sarcopenia. Wiley (2012/10/2)
http://as.wiley.com/WileyCDA/WileyTitle/productCd-1119975875.html
この書籍は発行が9月なのでまだかなり先ですが、著者は間違いないですし360ページの書籍ですので、かなり期待できると思います。内容はまだわかりませんが…。
ただ、どの書籍も老年医学のサルコペニアに関する内容がほとんどです。研究が老年医学領域で進んでいるので当たり前ではありますが…。今後、リハ栄養のサルコペニア(広義:廃用・飢餓・疾患を含む)の書籍も作らなければと感じています。
2012年3月23日金曜日
近森病院NST見学
昨日は、近森リハ病院リハ科の和田先生のお誘い(私の押し掛けかな)で、近森病院のNSTを見学させていただきました。
近森病院のNSTといえば、雑誌「臨床栄養」の最新号(2012年3月号)でも取り上げられていますように、極めて臨床栄養管理とリハの質が高い病院です。
http://www.ishiyaku.co.jp/magazines/eiyo/EiyoBookDetail.aspx?BC=061203
14時から近森正幸先生の参加されるNST回診を見学させていただきました。ICUとCCUに入院されている2人が対象でした。参加者職種は管理栄養士4-5人、薬剤師、看護師、臨床検査技師、理学療法士と、春休みで自主的に実習にきていた管理栄養士の学生(新4年生)4-5人でした。
2例であればそれほど時間がかからないのではと思うかもしれませんが、2時間以上かけていました。学生がいないときは若い管理栄養士にいろいろ説明しながら質問するようですが、昨日は学生への質問、説明が中心でした。内容的には病態と栄養をつなげる部分の解説が多かったです。
管理栄養士に限りませんが、若手の医療人はどうしても学校で学んだ知識というのは有機的に活用できません。学校教育の問題かもしれませんが。そこで、近森先生はいろんな知識をつなげて臨床現場で活躍できることを意識した、教育的NST回診を行っていました。
2例で2時間以上というのは質問される方も大変ですが、教える方も大変です。これを理事長・院長でありながら週2回行っているというのは、臨床栄養に対する情熱の現れです。栄養とリハがすべての医療の土台であり、ここをしっかり行うと回復が早くよくなることを繰り返し述べていました。私もまったく同感です。
このように管理栄養士を鍛えれば、3カ月で病棟に1人で配属可能(チューターに相談できる体制あり)、1年で1人前になるとのことでした。これだけ管理栄養士の卒後教育体制がしっかりしていれば、近森病院への就職を希望する管理栄養士が多いこともうなづけます。このような卒後教育システムを、日本中の管理栄養士に義務化すればよいのにと感じました。医師の臨床研修制度と同様にです。
夕方には、リハ栄養の講演をさせていただきました。近森病院では釈迦に説法のようなものでしたが、何とかやりました。若いスタッフにはリハ栄養の重要性を伝えることが少しはできたのではと思いますが、今回は私が学ぶことのほうがずっと多かったです。
講演後は近森先生や宮澤さんたちと、懇親会でこんな皿鉢料理をいただきました。食事はどれも美味しかったですし、ムルソーという白ワインをいただいたのですが、これもとても美味しかったです。おかげでだいぶ酔っ払いました(笑)。和田先生には二次会までお付き合いいただきました。
和田先生、近森先生、宮澤さんなど、多くの方に大変お世話になりました。本当にありがとうございました。今回の学びをリハ栄養の新たなコンセプト作りや生涯学習方法につなげたいと考えています。今後とも何卒よろしくお願い申し上げます。
2012年3月21日水曜日
人工透析患者の身体組成と死亡率
人工透析患者の身体組成代理マーカーによる死亡率予測に関する論文を紹介します。 人工透析患者のObesity Paradoxを説明できる論文です。
Kamyar Kalantar-Zadeh, Elani Streja, Miklos Z. Molnar, Lilia R. Lukowsky, Mahesh Krishnan, Csaba P. Kovesdy and Sander Greenland: Mortality Prediction by Surrogates of Body Composition: An Examination of the Obesity Paradox in Hemodialysis Patients Using Composite Ranking Score Analysis. Am. J. Epidemiol. (2012) doi: 10.1093/aje/kwr384 First published online: March 16, 2012
人工透析患者の死亡率と、dry weight(透析後体重)と血清クレアチニン値(筋肉量の代理マーカー)の変化との関連を、121,762人のコホートから後ろ向きに調査しています。
結果ですが、低体重、低筋肉量、体重減少、血清クレアチニン低下を認める場合、死亡率は高かったです。また、「体重減少・血清クレアチニン増加」した患者は、「体重増加・血清クレアチニン低下」した患者より、死亡率は低かったです。
これより体重減少より血清クレアチニン低下のほうがより強い死亡の予測因子といえます。人工透析患者のObesity Paradoxは、筋肉量減少の程度で説明できる可能性があるとしています。つまり、BMIに関わらず筋肉量が多い患者ほど死亡率が低くなるといえます。
Obesity Paradoxの論文はたくさんありますが、筋肉量である程度説明できるという論文は初めて見た気がします。人工透析患者(と腎機能正常の方)では血清クレアチニン値が筋肉量のマーカーであり、この数値と変化をみることで、一定の予後予測ができるかもしれませんね。
Abstract
In hemodialysis patients, lower body mass index and weight loss have been associated with higher mortality rates, a phenomenon sometimes called the obesity paradox. This apparent paradox might be explained by loss of muscle mass. The authors thus examined the relation to mortality of changes in dry weight and changes in serum creatinine levels (a muscle-mass surrogate) in a cohort of 121,762 hemodialysis patients who were followed for up to 5 years (2001–2006). In addition to conventional regression analyses, the authors conducted a ranking analysis of joint effects in which the sums and differences of the percentiles of change for the 2 measures in each patient were used as the regressors. Concordant with previous body mass index observations, lower body mass, lower muscle mass, weight loss, and serum creatinine decline were associated with higher death rates. Among patients with a discordant change, persons whose weight declined but whose serum creatinine levels increased had lower death rates than did those whose weight increased but whose serum creatinine level declined. A decline in serum creatinine appeared to be a stronger predictor of mortality than did weight loss. Assuming residual selection bias and confounding were not large, the present results suggest that a considerable proportion of the obesity paradox in dialysis patients might be explained by the amount of decline in muscle mass.
Kamyar Kalantar-Zadeh, Elani Streja, Miklos Z. Molnar, Lilia R. Lukowsky, Mahesh Krishnan, Csaba P. Kovesdy and Sander Greenland: Mortality Prediction by Surrogates of Body Composition: An Examination of the Obesity Paradox in Hemodialysis Patients Using Composite Ranking Score Analysis. Am. J. Epidemiol. (2012) doi: 10.1093/aje/kwr384 First published online: March 16, 2012
人工透析患者の死亡率と、dry weight(透析後体重)と血清クレアチニン値(筋肉量の代理マーカー)の変化との関連を、121,762人のコホートから後ろ向きに調査しています。
結果ですが、低体重、低筋肉量、体重減少、血清クレアチニン低下を認める場合、死亡率は高かったです。また、「体重減少・血清クレアチニン増加」した患者は、「体重増加・血清クレアチニン低下」した患者より、死亡率は低かったです。
これより体重減少より血清クレアチニン低下のほうがより強い死亡の予測因子といえます。人工透析患者のObesity Paradoxは、筋肉量減少の程度で説明できる可能性があるとしています。つまり、BMIに関わらず筋肉量が多い患者ほど死亡率が低くなるといえます。
Obesity Paradoxの論文はたくさんありますが、筋肉量である程度説明できるという論文は初めて見た気がします。人工透析患者(と腎機能正常の方)では血清クレアチニン値が筋肉量のマーカーであり、この数値と変化をみることで、一定の予後予測ができるかもしれませんね。
Abstract
In hemodialysis patients, lower body mass index and weight loss have been associated with higher mortality rates, a phenomenon sometimes called the obesity paradox. This apparent paradox might be explained by loss of muscle mass. The authors thus examined the relation to mortality of changes in dry weight and changes in serum creatinine levels (a muscle-mass surrogate) in a cohort of 121,762 hemodialysis patients who were followed for up to 5 years (2001–2006). In addition to conventional regression analyses, the authors conducted a ranking analysis of joint effects in which the sums and differences of the percentiles of change for the 2 measures in each patient were used as the regressors. Concordant with previous body mass index observations, lower body mass, lower muscle mass, weight loss, and serum creatinine decline were associated with higher death rates. Among patients with a discordant change, persons whose weight declined but whose serum creatinine levels increased had lower death rates than did those whose weight increased but whose serum creatinine level declined. A decline in serum creatinine appeared to be a stronger predictor of mortality than did weight loss. Assuming residual selection bias and confounding were not large, the present results suggest that a considerable proportion of the obesity paradox in dialysis patients might be explained by the amount of decline in muscle mass.
2012年3月20日火曜日
栄養とサルコペニアのレビュー
栄養とサルコペニアのレビュー論文を紹介します。
Siân Robinson, Cyrus Cooper, and Avan Aihie Sayer: Nutrition and Sarcopenia: A Review of the Evidence and Implications for Preventive Strategies. Journal of Aging Research Volume 2012 (2012), Article ID 510801, doi:10.1155/2012/510801
下記のHPで全文見ることができます。最近の論文まで含まれていて、サルコペニアの栄養療法の学習には有用だと思います。
http://www.hindawi.com/journals/jar/2012/510801/
サルコペニアの栄養療法として、蛋白、ビタミンD、抗酸化栄養素を十分摂取すべきとしています。n-3脂肪酸もサルコペニアに有効な可能性があります。ただし、観察研究による関連は確かでも、介入研究による有効性が検証されたものはわずかです。
運動と蛋白・アミノ酸の組み合わせに関しては、運動単独とそれほど変わらないという報告も少なくありません。もちろん有効という報告もありますが。低栄養やサルコペニアの高齢者ではより効果が高いのではと推測します。
サルコペニア予防を高齢になってから考えるのではなく、若年時の筋肉量のピークを高くすることで予防するという考え方があります。そのため生涯にわたる適切な食事と栄養が、サルコペニア予防の鍵となるかもしれません。
Abstract
Prevention of age-related losses in muscle mass and strength is key to protecting physical capability in older age and enabling independent living. To develop preventive strategies, a better understanding is needed of the lifestyle factors that influence sarcopenia and the mechanisms involved. Existing evidence indicates the potential importance of diets of adequate quality, to ensure sufficient intakes of protein, vitamin D, and antioxidant nutrients. Although much of this evidence is observational, the prevalence of low nutrient intakes and poor status among older adults make this a current concern. However, as muscle mass and strength in later life are a reflection of both the rate of muscle loss and the peak attained in early life, efforts to prevent sarcopenia also need to consider diet across the lifecourse and the potential effectiveness of early interventions. Optimising diet and nutrition throughout life may be key to preventing sarcopenia and promoting physical capability in older age.
Siân Robinson, Cyrus Cooper, and Avan Aihie Sayer: Nutrition and Sarcopenia: A Review of the Evidence and Implications for Preventive Strategies. Journal of Aging Research Volume 2012 (2012), Article ID 510801, doi:10.1155/2012/510801
下記のHPで全文見ることができます。最近の論文まで含まれていて、サルコペニアの栄養療法の学習には有用だと思います。
http://www.hindawi.com/journals/jar/2012/510801/
サルコペニアの栄養療法として、蛋白、ビタミンD、抗酸化栄養素を十分摂取すべきとしています。n-3脂肪酸もサルコペニアに有効な可能性があります。ただし、観察研究による関連は確かでも、介入研究による有効性が検証されたものはわずかです。
運動と蛋白・アミノ酸の組み合わせに関しては、運動単独とそれほど変わらないという報告も少なくありません。もちろん有効という報告もありますが。低栄養やサルコペニアの高齢者ではより効果が高いのではと推測します。
サルコペニア予防を高齢になってから考えるのではなく、若年時の筋肉量のピークを高くすることで予防するという考え方があります。そのため生涯にわたる適切な食事と栄養が、サルコペニア予防の鍵となるかもしれません。
Abstract
Prevention of age-related losses in muscle mass and strength is key to protecting physical capability in older age and enabling independent living. To develop preventive strategies, a better understanding is needed of the lifestyle factors that influence sarcopenia and the mechanisms involved. Existing evidence indicates the potential importance of diets of adequate quality, to ensure sufficient intakes of protein, vitamin D, and antioxidant nutrients. Although much of this evidence is observational, the prevalence of low nutrient intakes and poor status among older adults make this a current concern. However, as muscle mass and strength in later life are a reflection of both the rate of muscle loss and the peak attained in early life, efforts to prevent sarcopenia also need to consider diet across the lifecourse and the potential effectiveness of early interventions. Optimising diet and nutrition throughout life may be key to preventing sarcopenia and promoting physical capability in older age.
人工呼吸器管理と横隔膜機能不全
人工呼吸器管理では横隔膜の機能不全と萎縮を生じるというラットでの動物実験を紹介します。
Hudson, Matthew B, et al: Both high level pressure support ventilation and controlled mechanical ventilation induce diaphragm dysfunction and atrophy. Critical Care Medicine: April 2012 - Volume 40 - Issue 4 - p 1254–1260, doi: 10.1097/CCM.0b013e31823c8cc9
以前の研究でcontrolled mechanical ventilation(調節呼吸)によって、横隔膜の活動性が低下して、収縮機能障害と筋繊維萎縮で横隔膜の筋力低下が生じることがわかっています。
今回は、pressure support ventilation(圧サポート)では調節呼吸より、横隔膜の機能低下を少なくすることができるという仮説を検証するために動物実験を行いました。結果ですが、両者とも酸化ストレスと蛋白分解の活性化によって、横隔膜の機能低下を認めました。
ヒトでの研究ではないのでヒトでは該当しないかもしれませんが、人工呼吸器管理では横隔膜のサルコペニア(広義)が進む可能性があります。加齢、廃用、飢餓、疾患のすべての要素が重なり、呼吸筋のサルコペニアを認め、離脱困難となることも少なくないのではと思います。
Abstract
Objectives: Previous workers have demonstrated that controlled mechanical ventilation results in diaphragm inactivity and elicits a rapid development of diaphragm weakness as a result of both contractile dysfunction and fiber atrophy. Limited data exist regarding the impact of pressure support ventilation, a commonly used mode of mechanical ventilation—that permits partial mechanical activity of the diaphragm—on diaphragm structure and function. We carried out the present study to test the hypothesis that high-level pressure support ventilation decreases the diaphragm pathology associated with CMV.
Methods: Sprague-Dawley rats were randomly assigned to one of the following five groups:1) control (no mechanical ventilation); 2) 12 hrs of controlled mechanical ventilation (12CMV); 3) 18 hrs of controlled mechanical ventilation (18CMV); 4) 12 hrs of pressure support ventilation (12PSV); or 5) 18 hrs of pressure support ventilation (18PSV).
Measurements and Main Results: We carried out the following measurements on diaphragm specimens: 4-hydroxynonenal—a marker of oxidative stress, active caspase-3 (casp-3), active calpain-1 (calp-1), fiber type cross-sectional area, and specific force (sp F). Compared with the control, both 12PSV and 18PSV promoted a significant decrement in diaphragmatic specific force production, but to a lesser degree than 12CMV and 18CMV. Furthermore, 12CMV, 18PSV, and 18CMV resulted in significant atrophy in all diaphragm fiber types as well as significant increases in a biomarker of oxidative stress (4-hydroxynonenal) and increased proteolytic activity (20S proteasome, calpain-1, and caspase-3). Furthermore, although no inspiratory effort occurs during controlled mechanical ventilation, it was observed that pressure support ventilation resulted in large decrement, approximately 96%, in inspiratory effort compared with spontaneously breathing animals.
Conclusions: High levels of prolonged pressure support ventilation promote diaphragmatic atrophy and contractile dysfunction. Furthermore, similar to controlled mechanical ventilation, pressure support ventilation-induced diaphragmatic atrophy and weakness are associated with both diaphragmatic oxidative stress and protease activation. (Crit Care Med 2012; 40:–1260)
Hudson, Matthew B, et al: Both high level pressure support ventilation and controlled mechanical ventilation induce diaphragm dysfunction and atrophy. Critical Care Medicine: April 2012 - Volume 40 - Issue 4 - p 1254–1260, doi: 10.1097/CCM.0b013e31823c8cc9
以前の研究でcontrolled mechanical ventilation(調節呼吸)によって、横隔膜の活動性が低下して、収縮機能障害と筋繊維萎縮で横隔膜の筋力低下が生じることがわかっています。
今回は、pressure support ventilation(圧サポート)では調節呼吸より、横隔膜の機能低下を少なくすることができるという仮説を検証するために動物実験を行いました。結果ですが、両者とも酸化ストレスと蛋白分解の活性化によって、横隔膜の機能低下を認めました。
ヒトでの研究ではないのでヒトでは該当しないかもしれませんが、人工呼吸器管理では横隔膜のサルコペニア(広義)が進む可能性があります。加齢、廃用、飢餓、疾患のすべての要素が重なり、呼吸筋のサルコペニアを認め、離脱困難となることも少なくないのではと思います。
Abstract
Objectives: Previous workers have demonstrated that controlled mechanical ventilation results in diaphragm inactivity and elicits a rapid development of diaphragm weakness as a result of both contractile dysfunction and fiber atrophy. Limited data exist regarding the impact of pressure support ventilation, a commonly used mode of mechanical ventilation—that permits partial mechanical activity of the diaphragm—on diaphragm structure and function. We carried out the present study to test the hypothesis that high-level pressure support ventilation decreases the diaphragm pathology associated with CMV.
Methods: Sprague-Dawley rats were randomly assigned to one of the following five groups:1) control (no mechanical ventilation); 2) 12 hrs of controlled mechanical ventilation (12CMV); 3) 18 hrs of controlled mechanical ventilation (18CMV); 4) 12 hrs of pressure support ventilation (12PSV); or 5) 18 hrs of pressure support ventilation (18PSV).
Measurements and Main Results: We carried out the following measurements on diaphragm specimens: 4-hydroxynonenal—a marker of oxidative stress, active caspase-3 (casp-3), active calpain-1 (calp-1), fiber type cross-sectional area, and specific force (sp F). Compared with the control, both 12PSV and 18PSV promoted a significant decrement in diaphragmatic specific force production, but to a lesser degree than 12CMV and 18CMV. Furthermore, 12CMV, 18PSV, and 18CMV resulted in significant atrophy in all diaphragm fiber types as well as significant increases in a biomarker of oxidative stress (4-hydroxynonenal) and increased proteolytic activity (20S proteasome, calpain-1, and caspase-3). Furthermore, although no inspiratory effort occurs during controlled mechanical ventilation, it was observed that pressure support ventilation resulted in large decrement, approximately 96%, in inspiratory effort compared with spontaneously breathing animals.
Conclusions: High levels of prolonged pressure support ventilation promote diaphragmatic atrophy and contractile dysfunction. Furthermore, similar to controlled mechanical ventilation, pressure support ventilation-induced diaphragmatic atrophy and weakness are associated with both diaphragmatic oxidative stress and protease activation. (Crit Care Med 2012; 40:–1260)
Obesity Paradoxのレビュー
Obesity Paradoxのレビュー論文(Editorial)を紹介します。
Mitja Lainscak, Stephan von Haehling, Wolfram Doehner and Stefan D. Anker: The obesity paradox in chronic disease: facts and numbers. Journal of Cachexia, Sarcopenia and Muscle, Volume 3, Number 1, 1-4. doi: 10.1007/s13539-012-0059-5
下記のHPで全文見ることができます。
http://www.springerlink.com/content/504h421l33317812/fulltext.pdf
Obesity Paradoxは、心不全(急性、慢性)、冠動脈疾患(PCI、CABG後含め)、脳卒中、ICU領域、COPD(急性増悪、安定期)、CKD、DM+心疾患で報告されています。悪液質の原因疾患が多いですが、その他でも報告されつつあります。
健常者での最適なBMIと、特に慢性炎症性疾患の患者での最適なBMIは、異なる可能性があります。一次予防では肥満の場合、栄養療法と運動療法で体重減少をすすめるべきです。しかし、二次予防、三次予防では肥満の場合の対応をよく考えなければいけません。
Abstract
Body size, particularly large, is a matter of concern among the lay public. Whether this is justified depends upon the state of health and should be judged individually. For patients with established chronic disease, there is sufficient evidence to support the benefits of large body size, i.e., the obesity paradox. This uniform finding is shared over a variety of cardiovascular, pulmonary, and renal diseases and is counterintuitive to the current concepts on ideal body weight. The scientific community has to increase the awareness about differences for optimal body size in health and disease. Simultaneously, clinicians have to be aware about body weight dynamics implications and should interpret the changes in the context of an underlying disease in order to implement the best available management.
Mitja Lainscak, Stephan von Haehling, Wolfram Doehner and Stefan D. Anker: The obesity paradox in chronic disease: facts and numbers. Journal of Cachexia, Sarcopenia and Muscle, Volume 3, Number 1, 1-4. doi: 10.1007/s13539-012-0059-5
下記のHPで全文見ることができます。
http://www.springerlink.com/content/504h421l33317812/fulltext.pdf
Obesity Paradoxは、心不全(急性、慢性)、冠動脈疾患(PCI、CABG後含め)、脳卒中、ICU領域、COPD(急性増悪、安定期)、CKD、DM+心疾患で報告されています。悪液質の原因疾患が多いですが、その他でも報告されつつあります。
健常者での最適なBMIと、特に慢性炎症性疾患の患者での最適なBMIは、異なる可能性があります。一次予防では肥満の場合、栄養療法と運動療法で体重減少をすすめるべきです。しかし、二次予防、三次予防では肥満の場合の対応をよく考えなければいけません。
Abstract
Body size, particularly large, is a matter of concern among the lay public. Whether this is justified depends upon the state of health and should be judged individually. For patients with established chronic disease, there is sufficient evidence to support the benefits of large body size, i.e., the obesity paradox. This uniform finding is shared over a variety of cardiovascular, pulmonary, and renal diseases and is counterintuitive to the current concepts on ideal body weight. The scientific community has to increase the awareness about differences for optimal body size in health and disease. Simultaneously, clinicians have to be aware about body weight dynamics implications and should interpret the changes in the context of an underlying disease in order to implement the best available management.
2012年3月19日月曜日
透析開始時の低栄養と死亡率
透析開始時の低栄養と血清アルブミン値は死亡率の独立した予測因子であるという10年間のコホート研究を紹介します。
Maria Chan, et al: Malnutrition (Subjective Global Assessment) Scores and Serum Albumin Levels, but not Body Mass Index Values, at Initiation of Dialysis are Independent Predictors of Mortality: A 10-Year Clinical Cohort Study. Journal of renal nutrition, http://dx.doi.org/10.1053/j.jrn.2011.11.002
リサーチクエスチョンは以下の通りです。
P:透析開始した患者で
E:低栄養、血清アルブミン値が低い場合、
C:栄養状態良好、血清アルブミン値が正常の場合と比較して、
O:死亡率が高い
研究デザインは後ろ向きコホート研究です。
結果ですが、透析導入後の生存期間の中央値は54.2か月(約4.5年)で、透析開始時に52.1%がSGAで低栄養と判定されました。高齢、末梢血管疾患、血清アルブミン低値、低栄養が独立した死亡の予測因子でした。一方、BMIは死亡と有意な関連を認めませんでした。
今回の研究ではObesity Paradoxを認めませんでしたが、SGAで低栄養であれば生命予後が悪いということは明らかになりました。血清アルブミン値は栄養指標とはいえませんが、予後指標としてはやはり有用です。サルコペニアの有無で死亡率が異なるかどうかを知りたいですね。
Objective
To examine the associations between demographic, clinical, lifestyle, and nutritional parameters at the start of dialysis and mortality, including the combined effects on nutritional parameters, which were seldom investigated in the literature.
Design
Ten-year retrospective clinical cohort study.
Setting
Dialysis unit of a metropolitan tertiary teaching hospital in Sydney, Australia.
Subjects
Incident dialysis patients (n = 167; hemodialysis, 57.5%; male, 61.7%; age, 65.3 ± 13.6 years; diabetic, 24.5%) who commenced on a planned dialysis program.
Methods
Associations were examined between all-cause mortality and baseline demographics, including age and gender; clinical and lifestyle characteristics, including glomerular filtration rate, smoking habits, presence of comorbidities (e.g., coronary artery disease, diabetes mellitus, and peripheral vascular disease); and nutritional parameters, including body mass index (BMI), serum albumin (s-albumin) levels, and subjective global assessment score (SGA). Associations with combination values for malnutrition, s-albumin (<3.3 vs. ≥3.3 g/dL), and BMI (<26 vs. ≥26 kg/m2) were also examined.
Results
Median survival was 54.2 months (interquartile range, 23 to 83), and 52.1% of patients were malnourished (SGA score B and C) at the start of dialysis. Advanced age (classified as >65 years, P < .0001), presence of peripheral vascular disease (P < .0001), reduced s-albumin levels (P = .01), and malnutrition scores (P = .02) independently predicted mortality. Being overweight and obese (BMI: ≥26 kg/m2) did not show any advantage on survival (P = .73). Being malnourished and overweight (or obese) was associated with a 3-fold increase in mortality risk (adjusted hazard ratio [HR], 2.96; 95% confidence interval [CI], 1.12 to 7.33; P = .02) compared with being well nourished with a BMI <26 kg/m2 (referent). Compared with being well nourished (SGA = A), being malnourished with normal or low s-albumin was associated with higher risk (HR, 2.06; 95% CI, 1.06 to 4.00; P = .03 and HR, 2.86; 95% CI, 1.65 to 4.94; P < .0001, respectively). There was no statistical difference between mortality risks through any combination of s-albumin and BMI values (P = .54).
Conclusion
Malnutrition and reduced s-albumin levels were found to be independent predictors of mortality, whereas being overweight and obese did not show protective effects.
Maria Chan, et al: Malnutrition (Subjective Global Assessment) Scores and Serum Albumin Levels, but not Body Mass Index Values, at Initiation of Dialysis are Independent Predictors of Mortality: A 10-Year Clinical Cohort Study. Journal of renal nutrition, http://dx.doi.org/10.1053/j.jrn.2011.11.002
リサーチクエスチョンは以下の通りです。
P:透析開始した患者で
E:低栄養、血清アルブミン値が低い場合、
C:栄養状態良好、血清アルブミン値が正常の場合と比較して、
O:死亡率が高い
研究デザインは後ろ向きコホート研究です。
結果ですが、透析導入後の生存期間の中央値は54.2か月(約4.5年)で、透析開始時に52.1%がSGAで低栄養と判定されました。高齢、末梢血管疾患、血清アルブミン低値、低栄養が独立した死亡の予測因子でした。一方、BMIは死亡と有意な関連を認めませんでした。
今回の研究ではObesity Paradoxを認めませんでしたが、SGAで低栄養であれば生命予後が悪いということは明らかになりました。血清アルブミン値は栄養指標とはいえませんが、予後指標としてはやはり有用です。サルコペニアの有無で死亡率が異なるかどうかを知りたいですね。
Objective
To examine the associations between demographic, clinical, lifestyle, and nutritional parameters at the start of dialysis and mortality, including the combined effects on nutritional parameters, which were seldom investigated in the literature.
Design
Ten-year retrospective clinical cohort study.
Setting
Dialysis unit of a metropolitan tertiary teaching hospital in Sydney, Australia.
Subjects
Incident dialysis patients (n = 167; hemodialysis, 57.5%; male, 61.7%; age, 65.3 ± 13.6 years; diabetic, 24.5%) who commenced on a planned dialysis program.
Methods
Associations were examined between all-cause mortality and baseline demographics, including age and gender; clinical and lifestyle characteristics, including glomerular filtration rate, smoking habits, presence of comorbidities (e.g., coronary artery disease, diabetes mellitus, and peripheral vascular disease); and nutritional parameters, including body mass index (BMI), serum albumin (s-albumin) levels, and subjective global assessment score (SGA). Associations with combination values for malnutrition, s-albumin (<3.3 vs. ≥3.3 g/dL), and BMI (<26 vs. ≥26 kg/m2) were also examined.
Results
Median survival was 54.2 months (interquartile range, 23 to 83), and 52.1% of patients were malnourished (SGA score B and C) at the start of dialysis. Advanced age (classified as >65 years, P < .0001), presence of peripheral vascular disease (P < .0001), reduced s-albumin levels (P = .01), and malnutrition scores (P = .02) independently predicted mortality. Being overweight and obese (BMI: ≥26 kg/m2) did not show any advantage on survival (P = .73). Being malnourished and overweight (or obese) was associated with a 3-fold increase in mortality risk (adjusted hazard ratio [HR], 2.96; 95% confidence interval [CI], 1.12 to 7.33; P = .02) compared with being well nourished with a BMI <26 kg/m2 (referent). Compared with being well nourished (SGA = A), being malnourished with normal or low s-albumin was associated with higher risk (HR, 2.06; 95% CI, 1.06 to 4.00; P = .03 and HR, 2.86; 95% CI, 1.65 to 4.94; P < .0001, respectively). There was no statistical difference between mortality risks through any combination of s-albumin and BMI values (P = .54).
Conclusion
Malnutrition and reduced s-albumin levels were found to be independent predictors of mortality, whereas being overweight and obese did not show protective effects.
歯の喪失とがんでの死亡の関連
高齢者における歯の喪失とがんでの死亡の関連をまとめた書籍の1章を紹介します。
Toshihiro Ansai and Yutaka Takata: Association Between Tooth Loss and Cancer Mortality in Elderly Individuals
下記のHPで全文見ることができます。
http://cdn.intechopen.com/pdfs/29454/InTech-Association_between_tooth_loss_and_cancer_mortality_in_elderly_individuals.pdf
結論として、歯の喪失と胃がん、肺がん、膵がんの関連を認めるという報告もありますが、全体的には、曖昧な状況です。関連を認める可能性がある要因として、慢性炎症、栄養、サルコペニア、脳活動、QOL、社会経済状況があげれらています。個人的には年齢の要素が大きい気もしますが。
サルコペニアに関する記載の部分だけ引用させていただきます。仮説レベルではありますが、口腔・咀嚼のサルコペニアによって、食欲、食事摂取量、ADLが低下する可能性はあります。以下、引用です。
Sarcopenia is defined as muscle power decline or decreased muscular volume with aging,
leading to decreased levels of basal metabolism and energy consumption by the whole
body, which results in lower energy intake and a decrease in synthesis of proteins in the
body. To the best of our knowledge, no study concerning the association between chewing
ability (tooth loss) and sarcopenia has been presented, though it is considered that elderly
individuals with sarcopenia may also develop the condition in the oral cavity region, which
has been supported by several reports. For example, subjects with stable occlusion, eg.,
Eichner index (EI; Eichner, 1955) Class A were shown unlikely to stumble (Yoshida, 2005).
EI, long used as an indicator of occlusal condition, are based on existing natural tooth
contacts between the maxilla and mandible in the bilateral premolar and molar regions.
Class A represents contact in all 4 support zones. Some reports have been presented
regarding associations between stable occlusion and physical fitness ability (Yamaga et al.,
2002), chewing ability and physical fitness (Takata et al., 2004), and walking speed and oral
function (Okada et al., 2011). In a recent longitudinal study of Japanese elderly subjects,
partial or complete loss of occlusion was associated with a decline in leg extensor power or
decrease in one-leg standing time with eyes open (Okuyama et al., 2011). Sarcopenia may
have a negative influence on both chewing ability and oral function. A Japanese survey of
elderly individuals (60 to 87 years old) reported that significant factors related to occlusal
power were handgrip strength in males, walking speed for 5 m in both genders, and body
muscle volume in females (Kono, 2009). These findings suggest the possibility that oral
sarcopenia induces a negative spiral of systemic health conditions including decreased levels
of appetite and activities of daily living, as well as deterioration of psychosomatic health
conditions, such as occurrence of depression, though the causal relationship remains unclear.
Toshihiro Ansai and Yutaka Takata: Association Between Tooth Loss and Cancer Mortality in Elderly Individuals
下記のHPで全文見ることができます。
http://cdn.intechopen.com/pdfs/29454/InTech-Association_between_tooth_loss_and_cancer_mortality_in_elderly_individuals.pdf
結論として、歯の喪失と胃がん、肺がん、膵がんの関連を認めるという報告もありますが、全体的には、曖昧な状況です。関連を認める可能性がある要因として、慢性炎症、栄養、サルコペニア、脳活動、QOL、社会経済状況があげれらています。個人的には年齢の要素が大きい気もしますが。
サルコペニアに関する記載の部分だけ引用させていただきます。仮説レベルではありますが、口腔・咀嚼のサルコペニアによって、食欲、食事摂取量、ADLが低下する可能性はあります。以下、引用です。
Sarcopenia is defined as muscle power decline or decreased muscular volume with aging,
leading to decreased levels of basal metabolism and energy consumption by the whole
body, which results in lower energy intake and a decrease in synthesis of proteins in the
body. To the best of our knowledge, no study concerning the association between chewing
ability (tooth loss) and sarcopenia has been presented, though it is considered that elderly
individuals with sarcopenia may also develop the condition in the oral cavity region, which
has been supported by several reports. For example, subjects with stable occlusion, eg.,
Eichner index (EI; Eichner, 1955) Class A were shown unlikely to stumble (Yoshida, 2005).
EI, long used as an indicator of occlusal condition, are based on existing natural tooth
contacts between the maxilla and mandible in the bilateral premolar and molar regions.
Class A represents contact in all 4 support zones. Some reports have been presented
regarding associations between stable occlusion and physical fitness ability (Yamaga et al.,
2002), chewing ability and physical fitness (Takata et al., 2004), and walking speed and oral
function (Okada et al., 2011). In a recent longitudinal study of Japanese elderly subjects,
partial or complete loss of occlusion was associated with a decline in leg extensor power or
decrease in one-leg standing time with eyes open (Okuyama et al., 2011). Sarcopenia may
have a negative influence on both chewing ability and oral function. A Japanese survey of
elderly individuals (60 to 87 years old) reported that significant factors related to occlusal
power were handgrip strength in males, walking speed for 5 m in both genders, and body
muscle volume in females (Kono, 2009). These findings suggest the possibility that oral
sarcopenia induces a negative spiral of systemic health conditions including decreased levels
of appetite and activities of daily living, as well as deterioration of psychosomatic health
conditions, such as occurrence of depression, though the causal relationship remains unclear.
2012年3月15日木曜日
World Stroke Academyの嚥下障害資料
World Stroke Academyの嚥下障害資料を紹介させていただきます。下記のHPで52ページのPost Stroke Dysphagiaに関する資料を見ることができます。2010年の文献が引用されていますので、比較的新しい資料だと思います。
http://world-stroke-academy.org/pdf/WSA_Dyspagia_learning_module.pdf
World Stroke AcademyはWorld Stroke Organisation (WSO)のプロジェクトで、脳卒中に関する自己学習をすることもできます。嚥下障害以外にも有益な資料があります
(For Professionalsの中に)。
http://world-stroke-academy.org/
脳卒中後の嚥下障害の資料ですが、Presbyphagia(老嚥)に関する記載もいくつかあります。ブログに掲載した図は、それぞれ7ページ、40ページに掲載されています。
最初の図はPresbyphagia(老嚥)に影響する要因が挙げられています。この中にはmuscle atrophy、つまりサルコペニアももちろんあります。また、原発性、二次性のPresbyphagia(老嚥)も記載されています。
2番目の図はPresbyphagia(老嚥)の問題、原因、管理(対応)に関して、コンパクトにまとまっています。ただ、管理は代償手段がほとんどで、舌や嚥下筋のレジスタンストレーニングについてはほとんど触れられていません。
ただ、脳卒中による嚥下障害の中でも、Presbyphagia(老嚥)に関する記載がきちんとあることは素晴らしいと思います。低栄養に関する記載もしっかりあります。日本でもPresbyphagia(老嚥)、サルコペニアの嚥下障害が早く普及してほしいですね。
加齢と口腔・咽頭・食道の運動機能
加齢と口腔・咽頭・食道の運動機能に関するレビュー論文を紹介します。presbyphagia(老嚥)のレビュー論文ともいえます。
JoAnne Robbins, Allison Duke Bridges, and Andrew Taylor: Oral, pharyngeal and esophageal motor function in aging. GI Motility online (2006) doi:10.1038/gimo39
下記のHPで全文見ることができますので、presbyphagia(老嚥)に関心のある方はぜひ読んでみてください。サルコペニアによる嚥下障害とかなり関連があります。
http://www.nature.com/gimo/contents/pt1/full/gimo39.html
この論文では何度もpresbyphagia(老嚥)という言葉が出てきます。また、presbyesophagus(老人性食道機能低下)という言葉も出てきます。これは1960年代に造られた言葉だそうです。
Weblio英和辞典でもpresbyesophagusは、加齢による食道括約筋の収縮力低下、老人性食道、老人食道という訳語があります。でもpresbyphagiaは登録されていないので、presbyesophagusのほうがメジャーな言葉かもしれません。
http://ejje.weblio.jp/content/presbyesophagus
Key Points
JoAnne Robbins, Allison Duke Bridges, and Andrew Taylor: Oral, pharyngeal and esophageal motor function in aging. GI Motility online (2006) doi:10.1038/gimo39
下記のHPで全文見ることができますので、presbyphagia(老嚥)に関心のある方はぜひ読んでみてください。サルコペニアによる嚥下障害とかなり関連があります。
http://www.nature.com/gimo/contents/pt1/full/gimo39.html
この論文では何度もpresbyphagia(老嚥)という言葉が出てきます。また、presbyesophagus(老人性食道機能低下)という言葉も出てきます。これは1960年代に造られた言葉だそうです。
Weblio英和辞典でもpresbyesophagusは、加齢による食道括約筋の収縮力低下、老人性食道、老人食道という訳語があります。でもpresbyphagiaは登録されていないので、presbyesophagusのほうがメジャーな言葉かもしれません。
http://ejje.weblio.jp/content/presbyesophagus
Key Points
- Presbyphagia refers to age-related changes in the oropharyngeal and esophageal swallowing of healthy adults.
- Sarcopenia is age-related loss of skeletal muscle mass, organization, and strength.
- Good health is maintained in the presence of disease-free presbyphagia.
- Healthy persons depend on a highly automated neuromuscular sensorimotor process that coordinates chewing, swallowing, and airway protection.
- Central and peripheral nervous system changes with age affect swallowing.
- Oropharyngeal swallowing changes with healthy aging:
- Slower
- Delayed onset of airway protection and upper esophageal sphincter (UES) opening
- Bolus adjacent to airway longer
- Reduced lingual pressures
- Esophageal swallowing changes with aging:
- Duration of esophageal peristalsis is prolonged and amplitude decreases (60–80 years).
- Esophageal contraction amplitude diminishes but function remains intact (80-90 years).
- Reduced frequency of secondary peristalsis
- Increased reflux events in elders
- Although compensatory interventions are traditional, exercise is promising to remediate and perhaps prevent decline in function.
リハ栄養と医学部卒前教育
今週から10月まで合計18回、水曜日の午前中に新6年生のリハ実習を担当することになりました。すべての医学部新6年生がリハ科を1週間ローテーションするのですが、その中で1コマ、リハ栄養のレクチャーも含めて行う予定です。
今まで一応、大学教員でありながらほとんど卒前教育に関与することはありませんでした。今回はじめて本格的に医学生の卒前教育に関与することになります。時間的にはかなり大変ですが…。
昨日はじめて担当しましたが、やはり栄養に関する授業はほとんどない(もしくは若干の授業はあったとしても医学生の記憶にはない)ことがわかりました。もちろん、優秀な学生ですので、栄養に関する基本的な知識は持っていました。
しかし、臨床栄養に関する知識はほとんど持っていませんでした。学ぶ機会がなかったので当然のことではありますが。病院内栄養不良、病院内での餓死、医師の臨床栄養に関する知識の乏しさ、NSTや臨床栄養管理の重要性を伝えるよい機会だと感じました。
また、機能訓練室では低栄養や過栄養の患者に機能訓練を行うことも少なくありませんので、その様子を見て診察してもらい、「栄養ケアなくしてリハなし」を実感してもらうのもよい機会だと思いました。
臨床栄養やリハ栄養を学ぶ機会は他にはないと思いますので、せめて「病院内で餓死させるような栄養管理をしてはいけない」、「栄養はリハのバイタルサインである」ことだけでも記憶に残るような実習にしたいと考えています。
今まで一応、大学教員でありながらほとんど卒前教育に関与することはありませんでした。今回はじめて本格的に医学生の卒前教育に関与することになります。時間的にはかなり大変ですが…。
昨日はじめて担当しましたが、やはり栄養に関する授業はほとんどない(もしくは若干の授業はあったとしても医学生の記憶にはない)ことがわかりました。もちろん、優秀な学生ですので、栄養に関する基本的な知識は持っていました。
しかし、臨床栄養に関する知識はほとんど持っていませんでした。学ぶ機会がなかったので当然のことではありますが。病院内栄養不良、病院内での餓死、医師の臨床栄養に関する知識の乏しさ、NSTや臨床栄養管理の重要性を伝えるよい機会だと感じました。
また、機能訓練室では低栄養や過栄養の患者に機能訓練を行うことも少なくありませんので、その様子を見て診察してもらい、「栄養ケアなくしてリハなし」を実感してもらうのもよい機会だと思いました。
臨床栄養やリハ栄養を学ぶ機会は他にはないと思いますので、せめて「病院内で餓死させるような栄養管理をしてはいけない」、「栄養はリハのバイタルサインである」ことだけでも記憶に残るような実習にしたいと考えています。
2012年3月14日水曜日
第49回日本リハ医学会学術集会:栄養セッション
5月31日から6月2日まで第49回日本リハビリテーション医学会学術集会が福岡で開催されます。
http://www.congre.co.jp/jarm2012/index.html
まだプログラムとしては見ることはできませんが、今回、栄養のセッションが一般演題に2つありました。31日の午後に第8会場で、脳卒中(栄養1)と脳卒中(栄養2)があります。昨年の幕張のリハ学会では栄養のセッションがなくなってしまったのですが、今回復活してほっとしています。
私は脳卒中ではなく廃用症候群の栄養の研究ですが、脳卒中(栄養1)で発表させていただきます。同じセッションでお世話になっている百崎良先生、横山絵里子先生、湧上聖先生の発表があるようですので、とても楽しみです。
あと、まだ公開されていませんが、31日に「サルコペニア・
http://www.congre.co.jp/jarm2012/index.html
まだプログラムとしては見ることはできませんが、今回、栄養のセッションが一般演題に2つありました。31日の午後に第8会場で、脳卒中(栄養1)と脳卒中(栄養2)があります。昨年の幕張のリハ学会では栄養のセッションがなくなってしまったのですが、今回復活してほっとしています。
私は脳卒中ではなく廃用症候群の栄養の研究ですが、脳卒中(栄養1)で発表させていただきます。同じセッションでお世話になっている百崎良先生、横山絵里子先生、湧上聖先生の発表があるようですので、とても楽しみです。
あと、まだ公開されていませんが、31日に「サルコペニア・
リハ栄養ワークシート
病院家庭医を目指して~野望達成への道~のブログに、「リハ栄養ワークシート、作ってみました。」があります。
http://blog.livedoor.jp/gp_ken/archives/6830373.html
このブログの中で4ページのリハ栄養ワークシートが紹介されています。
http://www.scribd.com/doc/85196814/%E3%83%AA%E3%83%8F%E6%A0%84%E9%A4%8A%E3%83%AF%E3%83%BC%E3%82%AF%E3%82%B7%E3%83%BC%E3%83%88
分量は若干多いですが、一定の質以上のリハ栄養管理を実践するためには必須の項目がほとんどです。リハ栄養の基本を学ぶにも有用ですので、多くの方に見ていただければと思います。よろしくお願いいたします。
http://blog.livedoor.jp/gp_ken/archives/6830373.html
このブログの中で4ページのリハ栄養ワークシートが紹介されています。
http://www.scribd.com/doc/85196814/%E3%83%AA%E3%83%8F%E6%A0%84%E9%A4%8A%E3%83%AF%E3%83%BC%E3%82%AF%E3%82%B7%E3%83%BC%E3%83%88
分量は若干多いですが、一定の質以上のリハ栄養管理を実践するためには必須の項目がほとんどです。リハ栄養の基本を学ぶにも有用ですので、多くの方に見ていただければと思います。よろしくお願いいたします。
2012年3月13日火曜日
悪液質・疲労の包括的管理
悪液質と疲労に対する包括的・多職種協働の管理プログラムの総説論文を紹介します。
Watkins F, Tulloch S, Bennett C, Webster B, McCarthy C: A multimodal, interdisciplinary programme for the management of cachexia and fatigue. Int J Palliat Nurs. 2012 Feb;18(2):85-90.
抄録しか読めていませんが、悪液質・疲労の包括的管理の中身として、抗炎症薬(詳細不明です)、高蛋白摂取、個々にあわせたレジスタンストレーニングが挙げられています。
すでに病院、診療所では緩和ケアで、悪液質・疲労の包括的管理が成果を出していますが、今回は在宅で悪液質・疲労の包括的管理を行う取り組みが紹介されているようです。
抗炎症薬(詳細不明です)、高蛋白摂取、個々にあわせたレジスタンストレーニングの組み合わせというのは、まさに悪液質に対するリハ栄養管理です。不応性悪液質でなければ、つまり前悪液質、悪液質であれば、適切な栄養管理下でのレジスタンストレーニングは標準プログラムに入っています。
ただ、抗炎症薬と高蛋白摂取には個々にあわせてと書いてありませんが、レジスタンストレーニングだけは個々にあわせてと書いてあります。それだけ適切なリハ栄養評価のもとで実施することが重要だと考えます。日本でも悪液質・疲労の包括的管理を早く標準化したいですね。
Abstract
Fatigue and cachexia are common symptoms of advanced disease that have a significant impact on quality of life for palliative care clients. Management of cachexia and fatigue is often overlooked, but growing understanding of the multidimensional nature of fatigue and muscle wasting has led to interest in a model of care based on multimodal therapy that has been successfully implemented in specialized multidisciplinary hospital-based clinics in the oncology/palliative care setting. This article reports on an innovative incorporation of features of this model into a client-centred, interdisciplinary programme that aims to manage the effects of cachexia and fatigue and to improve quality of life for palliative care clients in their home setting. This Cachexia and Fatigue Management Programme (CFMP) involves the use of an anti-inflammatory agent, high protein intake, and an individually tailored resistance exercise regimen to counteract muscle wasting and fatigue. The article provides an overview of the role of multimodal therapies in the management of cachexia and fatigue before moving on to discuss the development of the CFMP, its features, and potential benefits for palliative care clients, caregivers, and health services.
Watkins F, Tulloch S, Bennett C, Webster B, McCarthy C: A multimodal, interdisciplinary programme for the management of cachexia and fatigue. Int J Palliat Nurs. 2012 Feb;18(2):85-90.
抄録しか読めていませんが、悪液質・疲労の包括的管理の中身として、抗炎症薬(詳細不明です)、高蛋白摂取、個々にあわせたレジスタンストレーニングが挙げられています。
すでに病院、診療所では緩和ケアで、悪液質・疲労の包括的管理が成果を出していますが、今回は在宅で悪液質・疲労の包括的管理を行う取り組みが紹介されているようです。
抗炎症薬(詳細不明です)、高蛋白摂取、個々にあわせたレジスタンストレーニングの組み合わせというのは、まさに悪液質に対するリハ栄養管理です。不応性悪液質でなければ、つまり前悪液質、悪液質であれば、適切な栄養管理下でのレジスタンストレーニングは標準プログラムに入っています。
ただ、抗炎症薬と高蛋白摂取には個々にあわせてと書いてありませんが、レジスタンストレーニングだけは個々にあわせてと書いてあります。それだけ適切なリハ栄養評価のもとで実施することが重要だと考えます。日本でも悪液質・疲労の包括的管理を早く標準化したいですね。
Abstract
Fatigue and cachexia are common symptoms of advanced disease that have a significant impact on quality of life for palliative care clients. Management of cachexia and fatigue is often overlooked, but growing understanding of the multidimensional nature of fatigue and muscle wasting has led to interest in a model of care based on multimodal therapy that has been successfully implemented in specialized multidisciplinary hospital-based clinics in the oncology/palliative care setting. This article reports on an innovative incorporation of features of this model into a client-centred, interdisciplinary programme that aims to manage the effects of cachexia and fatigue and to improve quality of life for palliative care clients in their home setting. This Cachexia and Fatigue Management Programme (CFMP) involves the use of an anti-inflammatory agent, high protein intake, and an individually tailored resistance exercise regimen to counteract muscle wasting and fatigue. The article provides an overview of the role of multimodal therapies in the management of cachexia and fatigue before moving on to discuss the development of the CFMP, its features, and potential benefits for palliative care clients, caregivers, and health services.
2012年3月12日月曜日
臨床看護2012年3月臨時増刊号
臨床看護2012年3月臨時増刊号で、「これからの栄養管理を考える-経管栄養の知識とトラブル対策」が特集されています。
http://www.herusu-shuppan.co.jp/rinsho/rz201203.html
クローバーホスピタルの望月弘彦先生が企画・構成をされた力作です。私も「摂食・嚥下障害患者への経管栄養(1)医療の実際」を執筆させていただきました。
下記の目次を見ていただければわかりますが、内容、執筆陣とも充実していると思います。多くの方に読んでいただければと思います。よろしくお願いいたします。
目次
望月 弘彦(クローバーホスピタル消化器科)
1 栄養評価
亀井 尚(東北大学大学院医学系研究科外科病態学講座),他
2 経腸栄養管理における必要栄養量の設定について
栗原 美香(滋賀医科大学附属病院栄養治療部),他
3 消化と吸収
雨海 照祥(武庫川女子大学生活環境学部食物栄養学科)
4 経管栄養の利点と適応
丸山 道生(東京都保健医療公社大久保病院)
5 経管栄養の種類と特徴
鷲澤 尚宏(東邦大学医療センター大森病院栄養治療センター)
6 経腸栄養の種類と選択のポイント
田中 弥生(駒沢女子大学人間健康学部)
1 経鼻経管栄養
森 みさ子(聖マリアンナ医科大学横浜市西部病院看護部)
2 PEGの適応と禁忌
伊藤 明彦(草津総合病院臨床栄養センター)
3 胃瘻造設手技
小野川 靖二(JA尾道総合病院)
4 PEG造設直後の管理
小川 哲史(前橋赤十字病院)
5 胃瘻の構造とカテーテルの種類
合田 文則(香川大学医学部附属病院腫瘍センター)
6 PEG術後のスキンケア
松原 康美(北里大学東病院看護部)
7 PEGの晩期合併症
有本 之嗣(須波宗斉会病院)
8 胃瘻カテーテル交換
倉 敏郎(町立長沼病院)
9 経皮経食道胃管挿入術(PTEG/ピーテグ)
大石 英人(東京女子医科大学八千代医療センター)
10 空腸瘻
丸山 道生(東京都保健医療公社大久保病院)
1 口腔ケア(Oral Health Care)について
石井 良昌(海老名総合病院)
2 栄養剤投与時の注意点
野田 さおり(KKR高松病院看護部)
3 経管栄養で用いられる器具の管理
鷲澤 尚宏(東邦大学医療センター大森病院栄養治療センター)
4 代謝性合併症とモニタリング
大村 健二(山中温泉医療センター)
5 胃瘻からの半固形化栄養材短時間注入法
合田 文則(香川大学医学部附属病院腫瘍センター)
6 薬剤投与
倉田 なおみ(昭和大学薬学部薬剤学教室)
1 摂食・嚥下障害患者への経管栄養
(1)医療の実際
若林 秀隆(横浜市立大学附属市民総合医療センターリハビリテーション科)
(2)看護の実際
上野 理美子(横浜市立大学附属市民総合医療センターリハビリテーション部)
2 糖尿病患者への経管栄養
(1)医療の実際
谷亀 光則(東海大学医学部腎代謝内科)
(2)看護の実際
坂根 絢子(東海大学医学部付属病院看護部)
3 腎不全患者への経管栄養
(1)医療の実際
安藤 亮一(武蔵野赤十字病院)
(2)看護の実際
飯塚 久子(武蔵野赤十字病院看護部)
4 肝臓病(肝硬変)患者への経管栄養
(1)医療の実際
加藤 章信(盛岡市立病院),他
(2)看護の実際
川代 千恵子(岩手医科大学附属病院看護部)
5 COPD患者への経管栄養
(1)医療の実際
粟井 一哉(KKR高松病院)
(2)看護の実際
稲木 美香(KKR高松病院看護部)
6 ALS患者への胃瘻造設と経管栄養
(1)医療の実際
清水 俊夫(東京都立神経病院)
(2)看護の実際
新井 玉南(東京都立神経病院看護科),他
7 認知症患者への経管栄養
(1)医療の実際
鈴木 裕(国際医療福祉大学病院)
(2)看護の実際
上野 優美(横浜市立みなと赤十字病院看護部),他
8 脳卒中患者への経管栄養
(1)医療の実際
三原 千惠(海老名総合病院附属海老名メディカルサポートセンター)
(2)看護の実際
佐々木奈津恵(海老名総合病院看護部),他
9 褥瘡のある患者への経管栄養
(1)医療の実際
岡田 晋吾(北美原クリニック)
(2)看護の実際
仙石 真由美(函館五稜郭病院看護部)
10 悪性腫瘍の患者への経管栄養
(1)医療の実際
峯 真司(がん研有明病院),他
(2)看護の実際
髙瀬 鮎美(がん研有明病院看護部),他
11 小児患者への経管栄養
(1)医療の実際
高増 哲也(神奈川県立こども医療センター)
(2)看護の実際
吉橋 恭子(神奈川県立こども医療センター看護局)
12 小児外科と周術期経腸栄養管理
(1)医療の実際
千葉 正博(昭和大学藤が丘病院),他
(2)看護の実際
岩井 祐介(昭和大学藤が丘病院看護部),他
1 療養環境における違い (1)ICUにおける経腸栄養
松田 直之(名古屋大学大学院医学系研究科救急・集中治療医学分野)
(2)Immunonutrition
大竹 美緒(山梨大学医学部附属病院看護部),他
(3)急性期病院における経管栄養
井谷 智尚(西神戸医療センター)
(4)慢性期病院における経管栄養
向井 淳子(クローバーホスピタル看護部),他
(5)介護施設における経管栄養
石塚 泉(石塚内科クリニック)
(6)在宅における経管栄養
小川 滋彦(小川医院)
(7)長期療養患者への経管栄養
長谷川 正光(刈谷豊田総合病院高浜分院)
2 下痢/逆流への対処
(1)エレンタールと胃内減圧
堀内 朗(昭和伊南総合病院消化器病センター)
(2)経腸栄養ポンプとOS-1(R)
宮澤 靖(近森病院臨床栄養部)
(3)半固形化
蟹江 治郎(ふきあげ内科胃腸科クリニック)
3 チームで取り組む経管栄養の安全対策:NST(Nutrition support team)
(1)医師の立場から
大原 寛之(藤田保健衛生大学),他
(2)看護師の立場から
添野 民江(昭和大学藤が丘病院看護部),他
(3)管理栄養士の立場から
田崎 亮子(KKR新別府病院栄養管理室・栄養サポート室)
(4)薬剤師の立場から
増田 修三(尾道市公立みつぎ総合病院地域医療部)
(5)臨床検査技師の立場から
後藤 薫(東京都立小児総合医療センター検査科)
4 在宅管理での多職種連携
(1)看護師の立場から
中村 悦子(市立輪島病院看護部)
(2)薬剤師の立場から
長谷川 聰(株式会社フレディタカノ薬局)
(3)管理栄養士の立場から
手塚 波子(小川医院)
(4)歯科の立場から
菊谷 武(日本歯科大学附属病院口腔介護・リハビリテーションセンター)
5 大規模震災時に経管栄養剤をどうするか?
田村 佳奈美(かとう内科クリニック)
http://www.herusu-shuppan.co.jp/rinsho/rz201203.html
クローバーホスピタルの望月弘彦先生が企画・構成をされた力作です。私も「摂食・嚥下障害患者への経管栄養(1)医療の実際」を執筆させていただきました。
下記の目次を見ていただければわかりますが、内容、執筆陣とも充実していると思います。多くの方に読んでいただければと思います。よろしくお願いいたします。
目次
特集にあたって
望月 弘彦(クローバーホスピタル消化器科)
経管栄養の考え方と,ナースが押さえておくべき基礎知識
1 栄養評価
亀井 尚(東北大学大学院医学系研究科外科病態学講座),他
2 経腸栄養管理における必要栄養量の設定について
栗原 美香(滋賀医科大学附属病院栄養治療部),他
3 消化と吸収
雨海 照祥(武庫川女子大学生活環境学部食物栄養学科)
4 経管栄養の利点と適応
丸山 道生(東京都保健医療公社大久保病院)
5 経管栄養の種類と特徴
鷲澤 尚宏(東邦大学医療センター大森病院栄養治療センター)
6 経腸栄養の種類と選択のポイント
田中 弥生(駒沢女子大学人間健康学部)
患者の安全を守るための経管栄養の知識
1 経鼻経管栄養
森 みさ子(聖マリアンナ医科大学横浜市西部病院看護部)
2 PEGの適応と禁忌
伊藤 明彦(草津総合病院臨床栄養センター)
3 胃瘻造設手技
小野川 靖二(JA尾道総合病院)
4 PEG造設直後の管理
小川 哲史(前橋赤十字病院)
5 胃瘻の構造とカテーテルの種類
合田 文則(香川大学医学部附属病院腫瘍センター)
6 PEG術後のスキンケア
松原 康美(北里大学東病院看護部)
7 PEGの晩期合併症
有本 之嗣(須波宗斉会病院)
8 胃瘻カテーテル交換
倉 敏郎(町立長沼病院)
9 経皮経食道胃管挿入術(PTEG/ピーテグ)
大石 英人(東京女子医科大学八千代医療センター)
10 空腸瘻
丸山 道生(東京都保健医療公社大久保病院)
経管栄養患者のケアの実際
1 口腔ケア(Oral Health Care)について
石井 良昌(海老名総合病院)
2 栄養剤投与時の注意点
野田 さおり(KKR高松病院看護部)
3 経管栄養で用いられる器具の管理
鷲澤 尚宏(東邦大学医療センター大森病院栄養治療センター)
4 代謝性合併症とモニタリング
大村 健二(山中温泉医療センター)
5 胃瘻からの半固形化栄養材短時間注入法
合田 文則(香川大学医学部附属病院腫瘍センター)
6 薬剤投与
倉田 なおみ(昭和大学薬学部薬剤学教室)
各疾患における経管栄養
1 摂食・嚥下障害患者への経管栄養
(1)医療の実際
若林 秀隆(横浜市立大学附属市民総合医療センターリハビリテーション科)
(2)看護の実際
上野 理美子(横浜市立大学附属市民総合医療センターリハビリテーション部)
2 糖尿病患者への経管栄養
(1)医療の実際
谷亀 光則(東海大学医学部腎代謝内科)
(2)看護の実際
坂根 絢子(東海大学医学部付属病院看護部)
3 腎不全患者への経管栄養
(1)医療の実際
安藤 亮一(武蔵野赤十字病院)
(2)看護の実際
飯塚 久子(武蔵野赤十字病院看護部)
4 肝臓病(肝硬変)患者への経管栄養
(1)医療の実際
加藤 章信(盛岡市立病院),他
(2)看護の実際
川代 千恵子(岩手医科大学附属病院看護部)
5 COPD患者への経管栄養
(1)医療の実際
粟井 一哉(KKR高松病院)
(2)看護の実際
稲木 美香(KKR高松病院看護部)
6 ALS患者への胃瘻造設と経管栄養
(1)医療の実際
清水 俊夫(東京都立神経病院)
(2)看護の実際
新井 玉南(東京都立神経病院看護科),他
7 認知症患者への経管栄養
(1)医療の実際
鈴木 裕(国際医療福祉大学病院)
(2)看護の実際
上野 優美(横浜市立みなと赤十字病院看護部),他
8 脳卒中患者への経管栄養
(1)医療の実際
三原 千惠(海老名総合病院附属海老名メディカルサポートセンター)
(2)看護の実際
佐々木奈津恵(海老名総合病院看護部),他
9 褥瘡のある患者への経管栄養
(1)医療の実際
岡田 晋吾(北美原クリニック)
(2)看護の実際
仙石 真由美(函館五稜郭病院看護部)
10 悪性腫瘍の患者への経管栄養
(1)医療の実際
峯 真司(がん研有明病院),他
(2)看護の実際
髙瀬 鮎美(がん研有明病院看護部),他
11 小児患者への経管栄養
(1)医療の実際
高増 哲也(神奈川県立こども医療センター)
(2)看護の実際
吉橋 恭子(神奈川県立こども医療センター看護局)
12 小児外科と周術期経腸栄養管理
(1)医療の実際
千葉 正博(昭和大学藤が丘病院),他
(2)看護の実際
岩井 祐介(昭和大学藤が丘病院看護部),他
経管栄養法の最前線
1 療養環境における違い (1)ICUにおける経腸栄養
松田 直之(名古屋大学大学院医学系研究科救急・集中治療医学分野)
(2)Immunonutrition
大竹 美緒(山梨大学医学部附属病院看護部),他
(3)急性期病院における経管栄養
井谷 智尚(西神戸医療センター)
(4)慢性期病院における経管栄養
向井 淳子(クローバーホスピタル看護部),他
(5)介護施設における経管栄養
石塚 泉(石塚内科クリニック)
(6)在宅における経管栄養
小川 滋彦(小川医院)
(7)長期療養患者への経管栄養
長谷川 正光(刈谷豊田総合病院高浜分院)
2 下痢/逆流への対処
(1)エレンタールと胃内減圧
堀内 朗(昭和伊南総合病院消化器病センター)
(2)経腸栄養ポンプとOS-1(R)
宮澤 靖(近森病院臨床栄養部)
(3)半固形化
蟹江 治郎(ふきあげ内科胃腸科クリニック)
3 チームで取り組む経管栄養の安全対策:NST(Nutrition support team)
(1)医師の立場から
大原 寛之(藤田保健衛生大学),他
(2)看護師の立場から
添野 民江(昭和大学藤が丘病院看護部),他
(3)管理栄養士の立場から
田崎 亮子(KKR新別府病院栄養管理室・栄養サポート室)
(4)薬剤師の立場から
増田 修三(尾道市公立みつぎ総合病院地域医療部)
(5)臨床検査技師の立場から
後藤 薫(東京都立小児総合医療センター検査科)
4 在宅管理での多職種連携
(1)看護師の立場から
中村 悦子(市立輪島病院看護部)
(2)薬剤師の立場から
長谷川 聰(株式会社フレディタカノ薬局)
(3)管理栄養士の立場から
手塚 波子(小川医院)
(4)歯科の立場から
菊谷 武(日本歯科大学附属病院口腔介護・リハビリテーションセンター)
5 大規模震災時に経管栄養剤をどうするか?
田村 佳奈美(かとう内科クリニック)
【コラム】:望月 弘彦(クローバーホスピタル消化器科)
-
◎胃瘻周囲の難治性びらんには軟膏の使い分けを
◎栄養が体を温める
◎右向き/左向き?
◎うまく伝えるためには天地人を考える
◎ココア、きなこ、発泡酒
2012年3月9日金曜日
presbyphagia(老嚥)の最初の論文
presbyphagia(老嚥、老人性嚥下機能低下)という言葉が最初に紹介されたと思われる論文を紹介します。
Jahnke V. [Dysphagia in the elderly]. HNO. 1991 Nov;39(11):442-4. [Article in German]
ドイツ語の論文ですので、もちろん抄録しか読んでいません…。dysphagia in the elderly ("presbyphagia") とありますが、今ではdysphagiaとpresbyphagiaは区別して考えます。
この抄録でも原発性presbyphagia(老嚥)と二次性presbyphagia(老嚥)のことが記載されています。加齢の要因しかない原発性presbyphagia(老嚥)と、疾患による二次性presbyphagia(老嚥)を鑑別しなければいけないとあります。
また、原発性presbyphagia(老嚥)より二次性presbyphagia(老嚥)のほうが高齢者にcommonとあります。1991年の時点ではそうだったかもしれませんが、2012年の時点では逆転している可能性があります。
サルコペニアという言葉が最初に紹介されたのは1988年です。それからわずか3年後にはpresbyphagia(老嚥)という言葉もありました。サルコペニア元年が2012年ですので、3年後の2015年までにはpresbyphagia(老嚥)元年が来るかもしれません(笑)。
Abstract
The prevalence of dysphagia in the elderly ("presbyphagia") is probably still underestimated, though this disorder represents a major geriatric problem; special attention is necessary to prevent malnutrition, dehydration and aspiration pneumonia. Primary presbyphagia due to physiological, age-related changes of the swallowing mechanism must be differentiated from secondary presbyphagia attributable to diseases which are more frequent in the elderly. Transnasal pharyngo-laryngo-fiberendoscopy, videofluoroscopy and the "modified barium swallow" are of particular value in the diagnostic approach to presbyphagia. The possibilities of treatment are limited. They are aimed at dietary adjustments, compensatory mechanisms based on the properties of the volume and consistency of the food, proper feeding position and help by other persons. Individual swallowing exercises by a speech therapist are particularly valuable. Surgical procedures for the treatment of underlying organic disorders are less often indicated in presbyphagia.
Jahnke V. [Dysphagia in the elderly]. HNO. 1991 Nov;39(11):442-4. [Article in German]
ドイツ語の論文ですので、もちろん抄録しか読んでいません…。dysphagia in the elderly ("presbyphagia") とありますが、今ではdysphagiaとpresbyphagiaは区別して考えます。
この抄録でも原発性presbyphagia(老嚥)と二次性presbyphagia(老嚥)のことが記載されています。加齢の要因しかない原発性presbyphagia(老嚥)と、疾患による二次性presbyphagia(老嚥)を鑑別しなければいけないとあります。
また、原発性presbyphagia(老嚥)より二次性presbyphagia(老嚥)のほうが高齢者にcommonとあります。1991年の時点ではそうだったかもしれませんが、2012年の時点では逆転している可能性があります。
サルコペニアという言葉が最初に紹介されたのは1988年です。それからわずか3年後にはpresbyphagia(老嚥)という言葉もありました。サルコペニア元年が2012年ですので、3年後の2015年までにはpresbyphagia(老嚥)元年が来るかもしれません(笑)。
Abstract
The prevalence of dysphagia in the elderly ("presbyphagia") is probably still underestimated, though this disorder represents a major geriatric problem; special attention is necessary to prevent malnutrition, dehydration and aspiration pneumonia. Primary presbyphagia due to physiological, age-related changes of the swallowing mechanism must be differentiated from secondary presbyphagia attributable to diseases which are more frequent in the elderly. Transnasal pharyngo-laryngo-fiberendoscopy, videofluoroscopy and the "modified barium swallow" are of particular value in the diagnostic approach to presbyphagia. The possibilities of treatment are limited. They are aimed at dietary adjustments, compensatory mechanisms based on the properties of the volume and consistency of the food, proper feeding position and help by other persons. Individual swallowing exercises by a speech therapist are particularly valuable. Surgical procedures for the treatment of underlying organic disorders are less often indicated in presbyphagia.
嚥下障害と低栄養の統合管理
嚥下障害と低栄養の統合管理(Integrated Management of Dysphagia and Malnutrition)に関する資料を紹介します。下記のHPで確認できます。
http://www.nestlenutrition-institute.org/resources/library/Free/conference-proceeding/eugms2011/Documents/CH-NES-037%20EUGMS%206pp%20SH_LR_single%20(2).pdf
これはSatellite Symposium Proceedings 7th EUGMS(European Union of Geriatric Medicine Society) Congressの資料です。以下の3つの項目が紹介されています。
Oropharyngeal dysphagia: A growing concern in healthcare
Pathophysiology, relevance, and natural history of oropharyngeal dysphagia among the elderly
Dysphagia and malnutrition: From screening to treatment
詳細は上記HPを参照していただき、ここでは3つの図を紹介します。
最初の図はpresbyphagia(老嚥、老人性嚥下機能低下)に関するものです。presbyphagiaに影響する要因の1つにサルコペニアが挙げられています。また、その他にも舌や嚥下の遅れはサルコペニアが関連している可能性があります。
2番目の図は嚥下障害患者の管理プロトコールです。ポイントは最初に嚥下スクリーニングとしてEAT-10が紹介されていることです。EAT-10は以下のブログを参照してください。
EAT-10による嚥下スクリーニング
EAT-10の特徴として、この資料では以下のように紹介されています。
the EAT-10 is:
• A useful self-administered test of 10 items
• Easy to understand for the majority (95.4%) of patients
• An analogical and direct-scored test, that is quick to perform
(mean administration time of <4 minutes)
• Useful for identifying patients at risk of dysphagia, with a clear
cut-off level (a score of ≥3 is abnormal)
脳卒中などで嚥下障害の存在が明らかな場合には、嚥下スクリーニングは不要で、最初からフードテストやVE、VFなどを行います。一方、presbyphagia(老嚥)の場合には、嚥下スクリーニングが必要です。適切な嚥下スクリーニングがなければ、presbyphagia(老嚥)を見落とす可能性があります。
低栄養の見落とし予防にはMNA-SFが有用だと考えていますが、presbyphagia(老嚥)の見落とし予防にはEAT-10が有用ではないかと私は感じています。presbyphagia(老嚥)、EAT-10とも今後、日本で広がってほしいと思います。
3番目の図は嚥下障害患者に対する栄養介入です。absolute dysphagiaは経口摂取不可能な重度の嚥下障害、relative dysphagiaは経口摂取可能な中等度~軽度の嚥下障害のようです。いずれにしても適切な栄養管理が必要です。
2012年3月8日木曜日
高齢者の嚥下障害:presbyphagia
高齢者の嚥下障害に関するレビュー論文を紹介します。ここでもpresbyphagia(老人性嚥下機能低下、老嚥)が出てきます。
Humbert IA, Robbins J. Dysphagia in the elderly. Phys Med Rehabil Clin N Am. 2008 Nov;19(4):853-66, ix-x.
下記のHPで全文見ることができます。
http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3182519/pdf/nihms79128.pdf
論文の中にPresbyphagia versus Dysphagiaという項目があります。やや長いですがこの部分を以下、引用します。
Although the anatomical, physiological, psychological and functional changes that occur in the dynamic process we refer to as “aging” place older adults at risk for dysphagia; a healthy older adult’s swallow is not inherently impaired. Presbyphagia refers to characteristic changes in the swallowing mechanism of otherwise healthy older adults. Clinicians are becoming more aware of the need to distinguish among dysphagia, presbyphagia (an old, yet healthy, swallow) and other related diagnoses in order to avoid over diagnosing and over treating dysphagia. With the increased threat of acute illness, multiple medications, and any number of age-related conditions, older adults are more vulnerable and can cross the line from a healthy older swallow to a person with dysphagia in association with certain perturbations including acute illness, surgery, chemo radiation and other factors. Previous work has focused primarily on the anatomy and physiology of the oropharyngeal swallowing mechanism. Age effects on the temporal evolution of isometric and swallowing pressure indicate a progression of change that, when combined with naturally diminished functional reserve (the resilient ability of the body to adapt to physiological stress make the older population more susceptible to dysphagia. We review age-related changes in peripheral and central nervous system control of head and neck structures for swallowing in this paper. In addition, we briefly discuss promising strategies for neurorehabilitation of
dysphagia that are based upon the recognition that swallowing disruption may, in part, be a manifestation of “sarcopenia”, the age-related loss of skeletal muscle mass, organization and strength as well as age-related changes in sensorimotor acuity and efficiency.
以上、引用です。Presbyphagiaは健常高齢者における加齢による嚥下機能変化とあります。そして、DysphagiaかPresbyphagiaかその他かを区別する必要性を、臨床家はより認識するようになったとあります。
急性疾患、手術、化学療法、放射線療法、複数の薬物療法、加齢に関連した状況などが生じることで、健常高齢者(原発性Presbyphagia)はより脆弱になり、嚥下障害(Dysphagia)に移行することがあります。
サルコペニアは主に四肢で研究されていますが、頭部や頚部の筋肉にも生じます。口腔、咀嚼、舌、嚥下の筋肉にも生じます。原発性Presbyphagia=原発性サルコペニアによる嚥下障害ではありませんが、強い関連があります。
サルコペニアによる嚥下障害やPresbyphagiaは、今までその重要性をあまり指摘されてきませんでした。確かにエビデンスは少ないですが、まったくないということはありません。どちらも研究は主に原発性で進んでいますが、臨床では二次性が多いです。
二次性Presbyphagiaは広義のサルコペニアによる嚥下障害と同様に、疾患の治療だけでなく、廃用予防(早期経口摂取)、栄養改善、舌や舌骨上筋群などレジスタンストレーニングの併用、つまりリハ栄養管理が機能改善に重要だと考えます。
Abstract
The capacity to swallow or eat is a basic human need and can be a great pleasure. Older adults look forward to sharing mealtimes and participating in social interactions. The loss of capacity to swallow and dine can have far-reaching implications. With age, the ability to swallow undergoes changes that increase the risk for disordered swallowing, with devastating health implications for older adults. With the growth in the aging population, dysphagia is becoming a national health care burden and concern. Upward of 40% of people in institutionalized settings are dysphagic. There is a need to address dysphagia in ambulatory, acute care, and long-term care settings.
Humbert IA, Robbins J. Dysphagia in the elderly. Phys Med Rehabil Clin N Am. 2008 Nov;19(4):853-66, ix-x.
下記のHPで全文見ることができます。
http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3182519/pdf/nihms79128.pdf
論文の中にPresbyphagia versus Dysphagiaという項目があります。やや長いですがこの部分を以下、引用します。
Although the anatomical, physiological, psychological and functional changes that occur in the dynamic process we refer to as “aging” place older adults at risk for dysphagia; a healthy older adult’s swallow is not inherently impaired. Presbyphagia refers to characteristic changes in the swallowing mechanism of otherwise healthy older adults. Clinicians are becoming more aware of the need to distinguish among dysphagia, presbyphagia (an old, yet healthy, swallow) and other related diagnoses in order to avoid over diagnosing and over treating dysphagia. With the increased threat of acute illness, multiple medications, and any number of age-related conditions, older adults are more vulnerable and can cross the line from a healthy older swallow to a person with dysphagia in association with certain perturbations including acute illness, surgery, chemo radiation and other factors. Previous work has focused primarily on the anatomy and physiology of the oropharyngeal swallowing mechanism. Age effects on the temporal evolution of isometric and swallowing pressure indicate a progression of change that, when combined with naturally diminished functional reserve (the resilient ability of the body to adapt to physiological stress make the older population more susceptible to dysphagia. We review age-related changes in peripheral and central nervous system control of head and neck structures for swallowing in this paper. In addition, we briefly discuss promising strategies for neurorehabilitation of
dysphagia that are based upon the recognition that swallowing disruption may, in part, be a manifestation of “sarcopenia”, the age-related loss of skeletal muscle mass, organization and strength as well as age-related changes in sensorimotor acuity and efficiency.
以上、引用です。Presbyphagiaは健常高齢者における加齢による嚥下機能変化とあります。そして、DysphagiaかPresbyphagiaかその他かを区別する必要性を、臨床家はより認識するようになったとあります。
急性疾患、手術、化学療法、放射線療法、複数の薬物療法、加齢に関連した状況などが生じることで、健常高齢者(原発性Presbyphagia)はより脆弱になり、嚥下障害(Dysphagia)に移行することがあります。
サルコペニアは主に四肢で研究されていますが、頭部や頚部の筋肉にも生じます。口腔、咀嚼、舌、嚥下の筋肉にも生じます。原発性Presbyphagia=原発性サルコペニアによる嚥下障害ではありませんが、強い関連があります。
サルコペニアによる嚥下障害やPresbyphagiaは、今までその重要性をあまり指摘されてきませんでした。確かにエビデンスは少ないですが、まったくないということはありません。どちらも研究は主に原発性で進んでいますが、臨床では二次性が多いです。
二次性Presbyphagiaは広義のサルコペニアによる嚥下障害と同様に、疾患の治療だけでなく、廃用予防(早期経口摂取)、栄養改善、舌や舌骨上筋群などレジスタンストレーニングの併用、つまりリハ栄養管理が機能改善に重要だと考えます。
Abstract
The capacity to swallow or eat is a basic human need and can be a great pleasure. Older adults look forward to sharing mealtimes and participating in social interactions. The loss of capacity to swallow and dine can have far-reaching implications. With age, the ability to swallow undergoes changes that increase the risk for disordered swallowing, with devastating health implications for older adults. With the growth in the aging population, dysphagia is becoming a national health care burden and concern. Upward of 40% of people in institutionalized settings are dysphagic. There is a need to address dysphagia in ambulatory, acute care, and long-term care settings.
presbyphagia(老嚥)とは
高齢者の嚥下障害評価のレビュー論文を紹介します。presbyphagia(老人性嚥下機能低下、略して老嚥)についても紹介します。
D. GINOCCHIO, E. BORGHI, A. SCHINDLER: Dysphagia assessment in the elderly. Nutritional Therapy & Metabolism / Vol. 27 no. 1, pp. 9-15
下記のHPで全文見ることができますので、サルコペニアの嚥下障害に関心のある方はぜひ読んでいただければと思います。
http://nutritional.wichtig.it/subs2009/vol.%2027%20no.%201%202009/9-15%20Ginocchio.pdf
サルコペニアの嚥下障害を考える上で、presbyphagiaは重要な概念です。presbyは老人、老年、phagiaは嚥下という意味です。定義としては健常高齢者における加齢による嚥下機能低下で、疾患による嚥下障害(dysphagia)とは異なります。
Wikipedia(英語版ですが)には、presbyphagiaの解説が載っています。
http://en.wikipedia.org/wiki/Presbyphagia
ただ、老人性嚥下機能低下では日本語として長いので、老眼と同じように老嚥と略すのがよいと思うのは私だけでしょうか・・・。私はpresbyphagiaの日本語訳を見たことがありません。ご存知の方がいらっしゃいましたら、教えていただけますでしょうか。
この論文では、primary presbyphagia(原発性老嚥)とsecondary presbyphagia(二次性老嚥)について解説しています。primary presbyphagiaは加齢以外に要因がないもの、secondary presbyphagiaは疾患による嚥下障害があるものを意味します。
これはサルコペニアにおける原発性(加齢以外に要因がないもの)と二次性(活動、栄養、疾患の要因があるもの)の分類に似ています。サルコペニア、presbyphagiaとも原発性は老年医学の概念、二次性はリハ、リハ栄養の概念となります。
リハ、リハ栄養で対象としているサルコペニア、presbyphagiaのほとんどは二次性です。ただ、原発性サルコペニアや原発性presbyphagiaを認める方に、何らかの疾患、侵襲、廃用、低栄養などが加わることで二次性となることは少なくないと思います。
原発性サルコペニアや原発性presbyphagiaであれば、舌筋力増強訓練や頭部挙上訓練などの筋力トレーニングで改善させることができます。そのため、高齢社会では原発性サルコペニアや原発性presbyphagiaの早期発見・治療が重要になります。
サルコペニアの嚥下障害=presbyphagiaとはいえませんが、かなり重複しています。例えば、舌や舌骨上筋群の筋肉量低下や筋力低下は重複しています。感覚低下はサルコペニアに含まれませんが、動きが遅いことは関連しているかもしれません。
リハ栄養で重要なのは、広義のサルコペニアによる嚥下障害や二次性presbyphagiaです。しかし、原発性サルコペニアによる嚥下障害や原発性presbyphagiaを理解することも大切だと考えます。
ABSTRACT:
Dysphagia becomes an increasingly common problem as people age; its prevalence and the increased risk of related complications (aspiration pneumonia, dehydration, malnutrition) has brought the attention of dysphagia specialists to the elderly. Dysphagia assessment in the elderly relies primarily on the same modalities as in other age groups: history, bedside examination, fiberoptic endoscopic examination of swallowing, and videofluoroscopy. However, the elderly often show differences in anatomy and physiology, as well as in the diseases presented and the environment in which they live; specialists involved in dysphagia assessment should take these specific aspects into consideration. Modification of swallowing simply related to aging is called primary presbyphagia, while swallowing impairment due to diseases in the elderly is called secondary presbyphagia. The main characteristics of deglutition and deglutition disorders in the elderly are thus reviewed here, with special emphasis on the assessment and decision-making implications specific for this patient category.
D. GINOCCHIO, E. BORGHI, A. SCHINDLER: Dysphagia assessment in the elderly. Nutritional Therapy & Metabolism / Vol. 27 no. 1, pp. 9-15
下記のHPで全文見ることができますので、サルコペニアの嚥下障害に関心のある方はぜひ読んでいただければと思います。
http://nutritional.wichtig.it/subs2009/vol.%2027%20no.%201%202009/9-15%20Ginocchio.pdf
サルコペニアの嚥下障害を考える上で、presbyphagiaは重要な概念です。presbyは老人、老年、phagiaは嚥下という意味です。定義としては健常高齢者における加齢による嚥下機能低下で、疾患による嚥下障害(dysphagia)とは異なります。
Wikipedia(英語版ですが)には、presbyphagiaの解説が載っています。
http://en.wikipedia.org/wiki/Presbyphagia
ただ、老人性嚥下機能低下では日本語として長いので、老眼と同じように老嚥と略すのがよいと思うのは私だけでしょうか・・・。私はpresbyphagiaの日本語訳を見たことがありません。ご存知の方がいらっしゃいましたら、教えていただけますでしょうか。
この論文では、primary presbyphagia(原発性老嚥)とsecondary presbyphagia(二次性老嚥)について解説しています。primary presbyphagiaは加齢以外に要因がないもの、secondary presbyphagiaは疾患による嚥下障害があるものを意味します。
これはサルコペニアにおける原発性(加齢以外に要因がないもの)と二次性(活動、栄養、疾患の要因があるもの)の分類に似ています。サルコペニア、presbyphagiaとも原発性は老年医学の概念、二次性はリハ、リハ栄養の概念となります。
リハ、リハ栄養で対象としているサルコペニア、presbyphagiaのほとんどは二次性です。ただ、原発性サルコペニアや原発性presbyphagiaを認める方に、何らかの疾患、侵襲、廃用、低栄養などが加わることで二次性となることは少なくないと思います。
原発性サルコペニアや原発性presbyphagiaであれば、舌筋力増強訓練や頭部挙上訓練などの筋力トレーニングで改善させることができます。そのため、高齢社会では原発性サルコペニアや原発性presbyphagiaの早期発見・治療が重要になります。
サルコペニアの嚥下障害=presbyphagiaとはいえませんが、かなり重複しています。例えば、舌や舌骨上筋群の筋肉量低下や筋力低下は重複しています。感覚低下はサルコペニアに含まれませんが、動きが遅いことは関連しているかもしれません。
リハ栄養で重要なのは、広義のサルコペニアによる嚥下障害や二次性presbyphagiaです。しかし、原発性サルコペニアによる嚥下障害や原発性presbyphagiaを理解することも大切だと考えます。
ABSTRACT:
Dysphagia becomes an increasingly common problem as people age; its prevalence and the increased risk of related complications (aspiration pneumonia, dehydration, malnutrition) has brought the attention of dysphagia specialists to the elderly. Dysphagia assessment in the elderly relies primarily on the same modalities as in other age groups: history, bedside examination, fiberoptic endoscopic examination of swallowing, and videofluoroscopy. However, the elderly often show differences in anatomy and physiology, as well as in the diseases presented and the environment in which they live; specialists involved in dysphagia assessment should take these specific aspects into consideration. Modification of swallowing simply related to aging is called primary presbyphagia, while swallowing impairment due to diseases in the elderly is called secondary presbyphagia. The main characteristics of deglutition and deglutition disorders in the elderly are thus reviewed here, with special emphasis on the assessment and decision-making implications specific for this patient category.
2012年3月7日水曜日
虚弱高齢者の嚥下障害の病態生理
虚弱高齢者の嚥下障害の病態生理に関する論文を紹介します。
Rofes L, Arreola V, Romea M, Palomera E, Almirall J, Cabré M, Serra-Prat M, Clavé P. Pathophysiology of oropharyngeal dysphagia in the frail elderly. Neurogastroenterol Motil. 2010 Aug;22(8):851-8, e230.
対象は70歳以上で急性期病院に入院して、V-VSTで嚥下障害があると判定された虚弱高齢者45人です。健康なボランティア(40歳)と比べて、嚥下機能をVFで調査しました。虚弱の診断にはFriedの基準を用いています(5%以上の体重減少、疲労、筋力低下、歩行速度低下、活動レベル低下の5項目のうち3項目以上に該当)。
その結果、虚弱高齢者では63%に咽頭残留、57%に喉頭侵入、17%に誤嚥を認めました。VFで安全な嚥下ができなかった虚弱高齢者は、安全な嚥下ができた虚弱高齢者と比較して、喉頭前庭閉鎖が遅く、食塊移送が弱く、身体能力が低く、1年後の死亡率が高かったです。
また、VFで咽頭残留を認めた虚弱高齢者は、舌による移送の障害、舌骨の動きの遅れ、1年後の高い死亡率を認めました。以上より、虚弱高齢者の嚥下障害の治療では、喉頭前庭閉鎖、舌による移送の障害、舌骨の動きの遅れをターゲットにすべきという結論です。
今回の虚弱高齢者のうち、麻痺による嚥下障害の方は半数以下だと推測します(入院理由は呼吸器疾患38.9%、神経疾患13.9%、感染症13.9%、心疾患11.1%、代謝疾患11.1%となっているため)。つまり、サルコペニアによる嚥下障害の方が少なくないと思われます。
そう考えると、舌や舌骨上筋群のサルコペニアで、舌による移送の障害や舌骨の動きの遅れが生じている可能性があります。虚弱高齢者では、舌や舌骨上筋群のレジスタンストレーニング(舌筋力増強訓練、頭部挙上訓練、嚥下おでこ体操)を含めたリハ栄養管理が、嚥下障害対策として重要かもしれません。
Abstract
BACKGROUND: Oropharyngeal dysphagia is a major complaint among the elderly. Our aim was to assess the pathophysiology of oropharyngeal dysphagia in frail elderly patients (FEP).
METHODS: A total of 45 FEP (81.5 +/- 1.1 years) with oropharyngeal dysphagia and 12 healthy volunteers (HV, 40 +/- 2.4 years) were studied using videofluoroscopy. Each subject's clinical records, signs of safety and efficacy of swallow, timing of swallow response, hyoid motion and tongue bolus propulsion forces were assessed.
KEY RESULTS: Healthy volunteers presented a safe and efficacious swallow, faster laryngeal closure (0.157 +/- 0.013 s) upper esophageal sphincter opening (0.200 +/- 0.011 s), and maximal vertical hyoid motion (0.310 +/- 0.048 s), and stronger tongue propulsion forces (22.16 +/- 2.54 mN) than FEP. By contrast, 63.63% of FEP presented oropharyngeal residue, 57.10%, laryngeal penetration and 17.14%, tracheobronchial aspiration. Frail elderly patients with impaired swallow safety showed delayed laryngeal vestibule (LV) closure (0.476 +/- 0.047 s), similar bolus propulsion forces, poor functional capacity and higher 1-year mortality rates (51.7%vs 13.3%, P = 0.021) than FEP with safe swallow. Frail elderly patients with oropharyngeal residue showed impaired tongue propulsion (9.00 +/- 0.10 mN), delayed maximal vertical hyoid motion (0.612 +/- 0.071 s) and higher (56.0%vs 15.8%, P = 0.012) 1-year mortality rates than those with efficient swallow.
CONCLUSION & INFERENCES: Frail elderly patients with oropharyngeal dysphagia presented poor outcome and high mortality rates. Impaired safety of deglutition and aspirations are mainly caused by delayed LV closure. Impaired efficacy and residue are mainly related to weak tongue bolus propulsion forces and slow hyoid motion. Treatment of dysphagia in FEP should be targeted to improve these critical events.
Rofes L, Arreola V, Romea M, Palomera E, Almirall J, Cabré M, Serra-Prat M, Clavé P. Pathophysiology of oropharyngeal dysphagia in the frail elderly. Neurogastroenterol Motil. 2010 Aug;22(8):851-8, e230.
対象は70歳以上で急性期病院に入院して、V-VSTで嚥下障害があると判定された虚弱高齢者45人です。健康なボランティア(40歳)と比べて、嚥下機能をVFで調査しました。虚弱の診断にはFriedの基準を用いています(5%以上の体重減少、疲労、筋力低下、歩行速度低下、活動レベル低下の5項目のうち3項目以上に該当)。
その結果、虚弱高齢者では63%に咽頭残留、57%に喉頭侵入、17%に誤嚥を認めました。VFで安全な嚥下ができなかった虚弱高齢者は、安全な嚥下ができた虚弱高齢者と比較して、喉頭前庭閉鎖が遅く、食塊移送が弱く、身体能力が低く、1年後の死亡率が高かったです。
また、VFで咽頭残留を認めた虚弱高齢者は、舌による移送の障害、舌骨の動きの遅れ、1年後の高い死亡率を認めました。以上より、虚弱高齢者の嚥下障害の治療では、喉頭前庭閉鎖、舌による移送の障害、舌骨の動きの遅れをターゲットにすべきという結論です。
今回の虚弱高齢者のうち、麻痺による嚥下障害の方は半数以下だと推測します(入院理由は呼吸器疾患38.9%、神経疾患13.9%、感染症13.9%、心疾患11.1%、代謝疾患11.1%となっているため)。つまり、サルコペニアによる嚥下障害の方が少なくないと思われます。
そう考えると、舌や舌骨上筋群のサルコペニアで、舌による移送の障害や舌骨の動きの遅れが生じている可能性があります。虚弱高齢者では、舌や舌骨上筋群のレジスタンストレーニング(舌筋力増強訓練、頭部挙上訓練、嚥下おでこ体操)を含めたリハ栄養管理が、嚥下障害対策として重要かもしれません。
Abstract
BACKGROUND: Oropharyngeal dysphagia is a major complaint among the elderly. Our aim was to assess the pathophysiology of oropharyngeal dysphagia in frail elderly patients (FEP).
METHODS: A total of 45 FEP (81.5 +/- 1.1 years) with oropharyngeal dysphagia and 12 healthy volunteers (HV, 40 +/- 2.4 years) were studied using videofluoroscopy. Each subject's clinical records, signs of safety and efficacy of swallow, timing of swallow response, hyoid motion and tongue bolus propulsion forces were assessed.
KEY RESULTS: Healthy volunteers presented a safe and efficacious swallow, faster laryngeal closure (0.157 +/- 0.013 s) upper esophageal sphincter opening (0.200 +/- 0.011 s), and maximal vertical hyoid motion (0.310 +/- 0.048 s), and stronger tongue propulsion forces (22.16 +/- 2.54 mN) than FEP. By contrast, 63.63% of FEP presented oropharyngeal residue, 57.10%, laryngeal penetration and 17.14%, tracheobronchial aspiration. Frail elderly patients with impaired swallow safety showed delayed laryngeal vestibule (LV) closure (0.476 +/- 0.047 s), similar bolus propulsion forces, poor functional capacity and higher 1-year mortality rates (51.7%vs 13.3%, P = 0.021) than FEP with safe swallow. Frail elderly patients with oropharyngeal residue showed impaired tongue propulsion (9.00 +/- 0.10 mN), delayed maximal vertical hyoid motion (0.612 +/- 0.071 s) and higher (56.0%vs 15.8%, P = 0.012) 1-year mortality rates than those with efficient swallow.
CONCLUSION & INFERENCES: Frail elderly patients with oropharyngeal dysphagia presented poor outcome and high mortality rates. Impaired safety of deglutition and aspirations are mainly caused by delayed LV closure. Impaired efficacy and residue are mainly related to weak tongue bolus propulsion forces and slow hyoid motion. Treatment of dysphagia in FEP should be targeted to improve these critical events.
サルコペニアは院内感染の予測因子
サルコペニアは急性期病院での院内感染の予測因子であることを調査した論文を紹介します。質は高くありませんが…。
Cosquéric G, Sebag A, Ducolombier C, Thomas C, Piette F, Weill-Engerer S. Sarcopenia is predictive of nosocomial infection in care of the elderly. Br J Nutr. 2006 Nov;96(5):895-901.
リサーチ・クエスチョンは以下の通りのはずです。ただし、論文では主に院内感染の有無でデータ解析しています。
P:急性期病院に入院した65歳以上の高齢者で
E:サルコペニアを認めると、
C:サルコペニアを認めなかった場合と比較して、
O:入院後3週間以内の院内感染の割合が高い
サルコペニアはDEXAによる筋肉量のみで診断しています。結果ですが、サルコペニアを認めると、2.1倍院内感染のリスクが高くなりました(有意差あり)。サルコペニアに該当したのは29人で、そのうち13人に院内感染を認めました。一方、サルコペニア非該当の73人で院内感染を認めたのは16人でした。
院内感染は呼吸器感染が最も多く44.8%、次が尿路感染34.5%でした。院内感染の有無で比較すると、院内感染あり群では、ADLの自立度が低く、嚥下障害が多く(20.7%対1.4%)、チューブ類が多いという結果でした。以上より、サルコペニアは急性期病院での院内感染の予測因子という結論です。
問題点ですが、まずデータ解析がコホート研究なのか症例対照研究なのかがわかりにくいです。両者が混ざった解析をしています。サルコペニアに何人該当したのかは本文になく、図から数えました。次に多変量解析をしていません。サルコペニアを認める高齢者に嚥下障害を多く認めるために、誤嚥性肺炎などの院内感染が多い可能性を肯定も否定もできません。
今回の入院患者では、腎不全、心不全、認知症が多かったそうです。少なくとも健常高齢者ではありませんので、サルコペニアの原因が原発性か疾患(侵襲や悪液質)による二次性かその他かもわかりません。それでもサルコペニアが院内感染の予測因子(3週間以内に44.8%に発症)という意義はあります。
サルコペニア→院内感染(肺炎含め)→侵襲でさらなるサルコペニアの悪化→嚥下障害の出現・悪化→誤嚥性肺炎→さらなるサルコペニアの悪化という悪循環の可能性もありえます。入院時から適切なリハ栄養管理でサルコペニアの悪化を防ぐことは重要です。特に早期離床、早期経口摂取が重要と考えます。
Abstract
Protein-energy malnutrition and nosocomial infection (NI) are frequent in elderly patients, and a causal link between the two has often been suggested. The aim of the present study was to identify the nutritional parameters predictive of NI in elderly patients. We assessed on admission 101 patients (sixty-six women, thirty-five men, aged over 65 years) admitted to an acute care of the elderly department. Sarcopenia was detected by dual-energy X-ray absorptiometry, with appendicular skeletal muscle mass expressed with respect to body area. Weight, BMI, albuminaemia, serum transthyretin and C-reactive protein values were also determined on admission, and known risk factors, such as functional dependence and invasive biomedical material, were also evaluated. After up to 3 weeks of hospitalisation, patients were classified according to whether they had developed an NI. After 3 weeks of hospitalisation, we found that twenty-nine patients had suffered an NI, occurring after a mean of 16.1 d. Patients who were sarcopenic on admission had a significantly higher risk of contracting an NI (relative risk 2.1, 95 % CI 1.1, 3.8). None of the other morphometric or biological parameters differed significantly between the two groups of patients on admission. Patients who experienced an NI were also more likely, on admission, to have a medical device (P=0.02 to P=0.001 depending on the device), to have swallowing problems (P=0.002) or to have restricted autonomy (P<0.01). Sarcopenia on admission to an acute care of the elderly unit, as measured by X-ray absorptiometry, was therefore associated with a doubled risk of NI during the first 3 weeks of hospitalisation.
Cosquéric G, Sebag A, Ducolombier C, Thomas C, Piette F, Weill-Engerer S. Sarcopenia is predictive of nosocomial infection in care of the elderly. Br J Nutr. 2006 Nov;96(5):895-901.
リサーチ・クエスチョンは以下の通りのはずです。ただし、論文では主に院内感染の有無でデータ解析しています。
P:急性期病院に入院した65歳以上の高齢者で
E:サルコペニアを認めると、
C:サルコペニアを認めなかった場合と比較して、
O:入院後3週間以内の院内感染の割合が高い
サルコペニアはDEXAによる筋肉量のみで診断しています。結果ですが、サルコペニアを認めると、2.1倍院内感染のリスクが高くなりました(有意差あり)。サルコペニアに該当したのは29人で、そのうち13人に院内感染を認めました。一方、サルコペニア非該当の73人で院内感染を認めたのは16人でした。
院内感染は呼吸器感染が最も多く44.8%、次が尿路感染34.5%でした。院内感染の有無で比較すると、院内感染あり群では、ADLの自立度が低く、嚥下障害が多く(20.7%対1.4%)、チューブ類が多いという結果でした。以上より、サルコペニアは急性期病院での院内感染の予測因子という結論です。
問題点ですが、まずデータ解析がコホート研究なのか症例対照研究なのかがわかりにくいです。両者が混ざった解析をしています。サルコペニアに何人該当したのかは本文になく、図から数えました。次に多変量解析をしていません。サルコペニアを認める高齢者に嚥下障害を多く認めるために、誤嚥性肺炎などの院内感染が多い可能性を肯定も否定もできません。
今回の入院患者では、腎不全、心不全、認知症が多かったそうです。少なくとも健常高齢者ではありませんので、サルコペニアの原因が原発性か疾患(侵襲や悪液質)による二次性かその他かもわかりません。それでもサルコペニアが院内感染の予測因子(3週間以内に44.8%に発症)という意義はあります。
サルコペニア→院内感染(肺炎含め)→侵襲でさらなるサルコペニアの悪化→嚥下障害の出現・悪化→誤嚥性肺炎→さらなるサルコペニアの悪化という悪循環の可能性もありえます。入院時から適切なリハ栄養管理でサルコペニアの悪化を防ぐことは重要です。特に早期離床、早期経口摂取が重要と考えます。
Abstract
Protein-energy malnutrition and nosocomial infection (NI) are frequent in elderly patients, and a causal link between the two has often been suggested. The aim of the present study was to identify the nutritional parameters predictive of NI in elderly patients. We assessed on admission 101 patients (sixty-six women, thirty-five men, aged over 65 years) admitted to an acute care of the elderly department. Sarcopenia was detected by dual-energy X-ray absorptiometry, with appendicular skeletal muscle mass expressed with respect to body area. Weight, BMI, albuminaemia, serum transthyretin and C-reactive protein values were also determined on admission, and known risk factors, such as functional dependence and invasive biomedical material, were also evaluated. After up to 3 weeks of hospitalisation, patients were classified according to whether they had developed an NI. After 3 weeks of hospitalisation, we found that twenty-nine patients had suffered an NI, occurring after a mean of 16.1 d. Patients who were sarcopenic on admission had a significantly higher risk of contracting an NI (relative risk 2.1, 95 % CI 1.1, 3.8). None of the other morphometric or biological parameters differed significantly between the two groups of patients on admission. Patients who experienced an NI were also more likely, on admission, to have a medical device (P=0.02 to P=0.001 depending on the device), to have swallowing problems (P=0.002) or to have restricted autonomy (P<0.01). Sarcopenia on admission to an acute care of the elderly unit, as measured by X-ray absorptiometry, was therefore associated with a doubled risk of NI during the first 3 weeks of hospitalisation.
加齢と嚥下障害:戦略と介入
以前にも紹介しましたが、加齢と嚥下障害:インパクト、戦略、介入に関するレビュー論文を紹介します。
Ney DM, Weiss JM, Kind AJ, Robbins J. Senescent swallowing: impact, strategies, and interventions. Nutr Clin Pract. 2009 Jun-Jul;24(3):395-413.
下記のHPで全文見ることができます。
http://www.ncbi.nlm.nih.gov/pmc/articles/PMC2832792/pdf/nihms178630.pdf
以前、同じ論文を紹介したブログは下記です。
サルコペニアと嚥下障害の論文
サルコペニアによる嚥下障害に関して、比較的詳しくコメントされているレビュー論文です。今回は別のパート(Dysphagia, Nutrition and Hydration)を引用紹介します。以下、引用です。
Dysphagia, Nutrition and Hydration
Dysphagia has a profound effect on nutritional status often resulting in malnutrition and dehydration and may compromise nutrient status as a result of diminished capacity to eat or drink, anorexia or fear of eating. When dysphagia occurs in the elderly population in tandem with sarcopenia, or loss of skeletal muscle mass and strength (46), the risk for malnutrition especially protein-energy malnutrition is increased (47). Consequences of the dysphagia malnutrition relationship include: weight loss, dehydration, muscle breakdown, fatigue, aspiration pneumonia, and a general decline in functional status. Moreover, a recent study identified swallowing problems and sarcopenia as predictive of nosocomial infections in hospitalized elderly patients (48). Increased morbidity and mortality are documented outcomes of undiagnosed or untreated dysphagia that have progressed to protein-energy malnutrition (49,50).
一部訳しますと、高齢者でサルコペニアとともに嚥下障害が生じると、低栄養のリスクが高くなります。嚥下障害と低栄養の結果、体重減少、脱水、筋肉分解、疲労、誤嚥性肺炎、身体機能低下がおこります。さらに、嚥下障害とサルコペニアは、高齢者の院内感染の予測因子です。未診断・未治療の嚥下障害では、合併症の罹患率や死亡率が高くなります。
サルコペニアによる嚥下障害という書き方はされていませんが、全身の筋肉にサルコペニアが生じれば、程度の差はあっても嚥下に関わる筋肉にもサルコペニアは生じます。サルコペニアによる嚥下障害の結果、誤嚥性肺炎となり、さらにサルコペニアによる嚥下障害が悪化するという悪循環も生じえます。
エビデンスはまだ少ないですが、サルコペニアによる嚥下障害と誤嚥性肺炎の悪循環というコンセプトをきちんとした形にしたいと考えています。時期尚早ではありますが、臨床現場には広義のサルコペニアによる嚥下障害患者が少なからずいますので、理解の枠組みから作りたいと思います。
そのためには、サルコペニアによる嚥下障害の診断基準が必要です。例えば、誤嚥を認める高齢者で、嚥下障害の明らかな器質的、心理的な原因がなく、麻痺がない場合、除外診断として広義のサルコペニアによる嚥下障害と推測するのはいかがでしょうか。麻痺とサルコペニアを合併することもありますが…。
Abstract
The risk for disordered oropharyngeal swallowing (dysphagia) increases with age. Loss of swallowing function can have devastating health implications, including dehydration, malnutrition, pneumonia, and reduced quality of life. Age-related changes increase risk for dysphagia. First, natural, healthy aging takes its toll on head and neck anatomy and physiologic and neural mechanisms underpinning swallowing function. This progression of change contributes to alterations in the swallowing in healthy older adults and is termed presbyphagia, naturally diminishing functional reserve. Second, disease prevalence increases with age, and dysphagia is a comorbidity of many age-related diseases and/or their treatments. Sensory changes, medication, sarcopenia, and age-related diseases are discussed herein. Recent findings that health complications are associated with dysphagia are presented. Nutrient requirements, fluid intake, and nutrition assessment for older adults are reviewed relative to dysphagia. Dysphagia screening and the pros and cons of tube feeding as a solution are discussed. Optimal intervention strategies for elders with dysphagia ranging from compensatory interventions to more rigorous exercise approaches are presented. Compelling evidence of improved functional swallowing and eating outcomes resulting from active rehabilitation focusing on increasing strength of head and neck musculature is provided. In summary, although oropharyngeal dysphagia may be life threatening, so are some of the traditional alternatives, particularly for frail, elderly patients. Although the state of the evidence calls for more research, this review indicates that the behavioral, dietary, and environmental modifications emerging in this past decade are compassionate, promising, and, in many cases, preferred alternatives to the always present option of tube feeding.
Ney DM, Weiss JM, Kind AJ, Robbins J. Senescent swallowing: impact, strategies, and interventions. Nutr Clin Pract. 2009 Jun-Jul;24(3):395-413.
下記のHPで全文見ることができます。
http://www.ncbi.nlm.nih.gov/pmc/articles/PMC2832792/pdf/nihms178630.pdf
以前、同じ論文を紹介したブログは下記です。
サルコペニアと嚥下障害の論文
サルコペニアによる嚥下障害に関して、比較的詳しくコメントされているレビュー論文です。今回は別のパート(Dysphagia, Nutrition and Hydration)を引用紹介します。以下、引用です。
Dysphagia, Nutrition and Hydration
Dysphagia has a profound effect on nutritional status often resulting in malnutrition and dehydration and may compromise nutrient status as a result of diminished capacity to eat or drink, anorexia or fear of eating. When dysphagia occurs in the elderly population in tandem with sarcopenia, or loss of skeletal muscle mass and strength (46), the risk for malnutrition especially protein-energy malnutrition is increased (47). Consequences of the dysphagia malnutrition relationship include: weight loss, dehydration, muscle breakdown, fatigue, aspiration pneumonia, and a general decline in functional status. Moreover, a recent study identified swallowing problems and sarcopenia as predictive of nosocomial infections in hospitalized elderly patients (48). Increased morbidity and mortality are documented outcomes of undiagnosed or untreated dysphagia that have progressed to protein-energy malnutrition (49,50).
一部訳しますと、高齢者でサルコペニアとともに嚥下障害が生じると、低栄養のリスクが高くなります。嚥下障害と低栄養の結果、体重減少、脱水、筋肉分解、疲労、誤嚥性肺炎、身体機能低下がおこります。さらに、嚥下障害とサルコペニアは、高齢者の院内感染の予測因子です。未診断・未治療の嚥下障害では、合併症の罹患率や死亡率が高くなります。
サルコペニアによる嚥下障害という書き方はされていませんが、全身の筋肉にサルコペニアが生じれば、程度の差はあっても嚥下に関わる筋肉にもサルコペニアは生じます。サルコペニアによる嚥下障害の結果、誤嚥性肺炎となり、さらにサルコペニアによる嚥下障害が悪化するという悪循環も生じえます。
エビデンスはまだ少ないですが、サルコペニアによる嚥下障害と誤嚥性肺炎の悪循環というコンセプトをきちんとした形にしたいと考えています。時期尚早ではありますが、臨床現場には広義のサルコペニアによる嚥下障害患者が少なからずいますので、理解の枠組みから作りたいと思います。
そのためには、サルコペニアによる嚥下障害の診断基準が必要です。例えば、誤嚥を認める高齢者で、嚥下障害の明らかな器質的、心理的な原因がなく、麻痺がない場合、除外診断として広義のサルコペニアによる嚥下障害と推測するのはいかがでしょうか。麻痺とサルコペニアを合併することもありますが…。
Abstract
The risk for disordered oropharyngeal swallowing (dysphagia) increases with age. Loss of swallowing function can have devastating health implications, including dehydration, malnutrition, pneumonia, and reduced quality of life. Age-related changes increase risk for dysphagia. First, natural, healthy aging takes its toll on head and neck anatomy and physiologic and neural mechanisms underpinning swallowing function. This progression of change contributes to alterations in the swallowing in healthy older adults and is termed presbyphagia, naturally diminishing functional reserve. Second, disease prevalence increases with age, and dysphagia is a comorbidity of many age-related diseases and/or their treatments. Sensory changes, medication, sarcopenia, and age-related diseases are discussed herein. Recent findings that health complications are associated with dysphagia are presented. Nutrient requirements, fluid intake, and nutrition assessment for older adults are reviewed relative to dysphagia. Dysphagia screening and the pros and cons of tube feeding as a solution are discussed. Optimal intervention strategies for elders with dysphagia ranging from compensatory interventions to more rigorous exercise approaches are presented. Compelling evidence of improved functional swallowing and eating outcomes resulting from active rehabilitation focusing on increasing strength of head and neck musculature is provided. In summary, although oropharyngeal dysphagia may be life threatening, so are some of the traditional alternatives, particularly for frail, elderly patients. Although the state of the evidence calls for more research, this review indicates that the behavioral, dietary, and environmental modifications emerging in this past decade are compassionate, promising, and, in many cases, preferred alternatives to the always present option of tube feeding.
健常高齢者の誤嚥・舌筋力・握力の関連
健常高齢者で誤嚥・舌筋力・握力の関連を調査した論文を紹介します。
Butler SG, et al: The Relationship of Aspiration Status With Tongue and Handgrip Strength in Healthy Older Adults. J Gerontol A Biol Sci Med Sci (2011) 66A (4): 452-458. doi: 10.1093/gerona/glq234
近年、潜在性(無症状)の誤嚥を地域在住の高齢者の約30%に認めるという報告があります(今回の論文と同じ著者の報告ですが)。今回のリサーチ・クエスチョンは、
P:健常高齢者で
E:誤嚥を認めると
C:誤嚥を認めない場合と比較して
O:舌筋力が弱い(握力が弱い)
です。対象は78人の地域在住健常高齢者で、VEで37%に誤嚥を認めました。
結果ですが、等尺性の舌筋力は前方、後方とも、誤嚥を認めた高齢者で有意に低かったです。同様に嚥下時の舌筋力も前方、後方とも、誤嚥を認めた高齢者で有意に低い結果でした。また、誤嚥の有無で握力には有意差を認めませんでしたが、舌筋力と握力には有意な関連を認めました(r =0.34)。
以上より、健常高齢者で舌筋力が弱いと誤嚥しやすい可能性があります。また、舌筋力と握力に関連を認めたことより、咽頭の筋力低下は全身の加齢による筋力低下を反映している可能性があるという結論です。
この論文ではサルコペニアという用語は1回しかでてきませんが、全身のサルコペニア(筋力も含めた広義です)を認めると、舌・咽頭にもサルコペニアを認めやすいことが伺われます。また、舌も含めた嚥下筋のサルコペニアが、誤嚥と関連していることが推測されます。
潜在性の誤嚥を地域在住の高齢者の約30%に認めますが、VEで誤嚥を認めれば摂食・嚥下障害ありと言ってよいのでしょうか。日本で65歳以上の高齢者は2012年で3000万人を超えます。単純計算ですが、約900万人に潜在性の誤嚥(摂食・嚥下障害)を認める可能性があります。
潜在性の誤嚥を地域在住の高齢者の約30%に認める原因は明らかになっていませんが、その原因の1つは嚥下筋のサルコペニアと考えます。健常高齢者の嚥下機能の評価と誤嚥への対応が今後、ますます求められる可能性があります。
Abstract
Background. Recently, subclinical aspiration has been identified in approximately 30% of community-dwelling older adults. Given that the tongue is a key component of the safe swallow, we hypothesized healthy older adults who aspirate will generate less tongue strength than adults who do not aspirate. Furthermore, as muscle weakness may reflect a global effect of aging, we further investigated whether tongue strength is correlated with handgrip strength.
Methods. We assessed 78 healthy community-dwelling older adults (M = 77.3 years, SD = 7.26) for aspiration status (37% aspirators) via flexible endoscopic evaluation of swallowing. Maximal isometric anterior and posterior tongue strength, anterior and posterior swallowing tongue strength, and maximum handgrip strength were measured.
Results. Isometric tongue strength was significantly lower in aspirators versus nonaspirators (p = .03) at both the anterior (463 vs 548 mmHg, respectively) and posterior lingual locations (285 vs 370 mmHg, respectively). Likewise, swallowing tongue strength was significantly lower in aspirators versus nonaspirators at both the anterior (270 vs 317 mmHg, respectively) and posterior lingual locations (220 vs 267 mmHg, respectively). There was no difference between aspirators and nonaspirators’ handgrip strength (p > .05), although handgrip strength was correlated with posterior tongue strength (r = .34, p = .005).
Conclusions. Lower anterior and posterior isometric and swallowing tongue strength were dependent on aspiration status. Lower lingual strength in healthy adults may predispose them to aspiration. The correlation between tongue and handgrip strength is consistent with the hypothesis that impaired oropharyngeal strength reflects global age-related declines in muscle strength.
Butler SG, et al: The Relationship of Aspiration Status With Tongue and Handgrip Strength in Healthy Older Adults. J Gerontol A Biol Sci Med Sci (2011) 66A (4): 452-458. doi: 10.1093/gerona/glq234
近年、潜在性(無症状)の誤嚥を地域在住の高齢者の約30%に認めるという報告があります(今回の論文と同じ著者の報告ですが)。今回のリサーチ・クエスチョンは、
P:健常高齢者で
E:誤嚥を認めると
C:誤嚥を認めない場合と比較して
O:舌筋力が弱い(握力が弱い)
です。対象は78人の地域在住健常高齢者で、VEで37%に誤嚥を認めました。
結果ですが、等尺性の舌筋力は前方、後方とも、誤嚥を認めた高齢者で有意に低かったです。同様に嚥下時の舌筋力も前方、後方とも、誤嚥を認めた高齢者で有意に低い結果でした。また、誤嚥の有無で握力には有意差を認めませんでしたが、舌筋力と握力には有意な関連を認めました(r =0.34)。
以上より、健常高齢者で舌筋力が弱いと誤嚥しやすい可能性があります。また、舌筋力と握力に関連を認めたことより、咽頭の筋力低下は全身の加齢による筋力低下を反映している可能性があるという結論です。
この論文ではサルコペニアという用語は1回しかでてきませんが、全身のサルコペニア(筋力も含めた広義です)を認めると、舌・咽頭にもサルコペニアを認めやすいことが伺われます。また、舌も含めた嚥下筋のサルコペニアが、誤嚥と関連していることが推測されます。
潜在性の誤嚥を地域在住の高齢者の約30%に認めますが、VEで誤嚥を認めれば摂食・嚥下障害ありと言ってよいのでしょうか。日本で65歳以上の高齢者は2012年で3000万人を超えます。単純計算ですが、約900万人に潜在性の誤嚥(摂食・嚥下障害)を認める可能性があります。
潜在性の誤嚥を地域在住の高齢者の約30%に認める原因は明らかになっていませんが、その原因の1つは嚥下筋のサルコペニアと考えます。健常高齢者の嚥下機能の評価と誤嚥への対応が今後、ますます求められる可能性があります。
Abstract
Background. Recently, subclinical aspiration has been identified in approximately 30% of community-dwelling older adults. Given that the tongue is a key component of the safe swallow, we hypothesized healthy older adults who aspirate will generate less tongue strength than adults who do not aspirate. Furthermore, as muscle weakness may reflect a global effect of aging, we further investigated whether tongue strength is correlated with handgrip strength.
Methods. We assessed 78 healthy community-dwelling older adults (M = 77.3 years, SD = 7.26) for aspiration status (37% aspirators) via flexible endoscopic evaluation of swallowing. Maximal isometric anterior and posterior tongue strength, anterior and posterior swallowing tongue strength, and maximum handgrip strength were measured.
Results. Isometric tongue strength was significantly lower in aspirators versus nonaspirators (p = .03) at both the anterior (463 vs 548 mmHg, respectively) and posterior lingual locations (285 vs 370 mmHg, respectively). Likewise, swallowing tongue strength was significantly lower in aspirators versus nonaspirators at both the anterior (270 vs 317 mmHg, respectively) and posterior lingual locations (220 vs 267 mmHg, respectively). There was no difference between aspirators and nonaspirators’ handgrip strength (p > .05), although handgrip strength was correlated with posterior tongue strength (r = .34, p = .005).
Conclusions. Lower anterior and posterior isometric and swallowing tongue strength were dependent on aspiration status. Lower lingual strength in healthy adults may predispose them to aspiration. The correlation between tongue and handgrip strength is consistent with the hypothesis that impaired oropharyngeal strength reflects global age-related declines in muscle strength.
2012年3月6日火曜日
筋力低下の長期の決定因子
筋力低下の長期の決定因子を、22年間のフォローアップ調査で評価したフィンランドの研究を紹介します。
Stenholm S, Tiainen K, Rantanen T, Sainio P, Heliövaara M, Impivaara O, Koskinen S. Long-term determinants of muscle strength decline: prospective evidence from the 22-year mini-Finland follow-up survey. J Am Geriatr Soc. 2012 Jan;60(1):77-85. doi: 10.1111/j.1532-5415.2011.03779.x. Epub 2011 Dec 28.
22年間のコホートというだけで、個人的には脱帽です。
地域在住の963人の男女(ベースラインでは30-73歳)を対象に、握力で筋力を評価しています。握力低下と関連するリスク因子、ライフスタイル、慢性疾患などを調査しました。その結果、中年期での重労働、過体重、喫煙、心血管疾患、高血圧症、糖尿病、喘息があると、握力は有意に低下しました。
また、顕著な体重減少、活動量の少ない生活、喫煙の継続、冠動脈疾患、その他の心血管疾患、糖尿病、慢性気管支炎、慢性腰痛、長期の心血管疾患、高血圧、喘息があると、より加速的な握力低下を認めました。これらの早期発見、介入を行うことで、将来のサルコペニアや障害予防につながる可能性があるという結論です。
当たり前ですが、適度な食事と運動と禁煙はサルコペニア予防に大事ですね(笑)。その上で心血管疾患、高血圧症、糖尿病、喘息といった疾患を可能な範囲で予防(一次~三次まで含めて)していくことが、サルコペニアの一次予防にもつながるかもしれません。
Abstract
OBJECTIVES: To examine long-term changes in handgrip strength and the factors predicting handgrip strength decline.
DESIGN: Longitudinal cohort study with 22 years of follow-up.
SETTING: Population-based Mini-Finland Health Examination Survey in Finland.
PARTICIPANTS: Nine hundred sixty-three men and women aged 30 to 73 at baseline.
MEASUREMENTS: Handgrip strength was measured using a handheld dynamometer at baseline and follow-up. Information on potential risk factors, namely lifestyle and chronic conditions, and their changes throughout the follow-up were based on health interviews.
RESULTS: Based on linear mixed-effect models, midlife physically strenuous work, excess body weight, smoking, cardiovascular disease, hypertension, diabetes mellitus, and asthma predicted muscle strength decline over 22 years of follow-up (P < .05 for all). In addition, pronounced weight loss, becoming physically sedentary, persistent smoking, incident coronary heart disease, other cardiovascular disease, diabetes mellitus, chronic bronchitis, chronic back syndrome, long-lasting cardiovascular disease, hypertension, and asthma were associated with accelerated handgrip strength decline (P < .05 for all).
CONCLUSION: Lifestyle and physical health earlier in life determine rate of muscle strength decline in old age. Efforts should be made to recognize persons at risk in a timely manner and target early interventions to middle-aged persons to slow down muscle strength decline and prevent future functional limitations and disability.
Stenholm S, Tiainen K, Rantanen T, Sainio P, Heliövaara M, Impivaara O, Koskinen S. Long-term determinants of muscle strength decline: prospective evidence from the 22-year mini-Finland follow-up survey. J Am Geriatr Soc. 2012 Jan;60(1):77-85. doi: 10.1111/j.1532-5415.2011.03779.x. Epub 2011 Dec 28.
22年間のコホートというだけで、個人的には脱帽です。
地域在住の963人の男女(ベースラインでは30-73歳)を対象に、握力で筋力を評価しています。握力低下と関連するリスク因子、ライフスタイル、慢性疾患などを調査しました。その結果、中年期での重労働、過体重、喫煙、心血管疾患、高血圧症、糖尿病、喘息があると、握力は有意に低下しました。
また、顕著な体重減少、活動量の少ない生活、喫煙の継続、冠動脈疾患、その他の心血管疾患、糖尿病、慢性気管支炎、慢性腰痛、長期の心血管疾患、高血圧、喘息があると、より加速的な握力低下を認めました。これらの早期発見、介入を行うことで、将来のサルコペニアや障害予防につながる可能性があるという結論です。
当たり前ですが、適度な食事と運動と禁煙はサルコペニア予防に大事ですね(笑)。その上で心血管疾患、高血圧症、糖尿病、喘息といった疾患を可能な範囲で予防(一次~三次まで含めて)していくことが、サルコペニアの一次予防にもつながるかもしれません。
Abstract
OBJECTIVES: To examine long-term changes in handgrip strength and the factors predicting handgrip strength decline.
DESIGN: Longitudinal cohort study with 22 years of follow-up.
SETTING: Population-based Mini-Finland Health Examination Survey in Finland.
PARTICIPANTS: Nine hundred sixty-three men and women aged 30 to 73 at baseline.
MEASUREMENTS: Handgrip strength was measured using a handheld dynamometer at baseline and follow-up. Information on potential risk factors, namely lifestyle and chronic conditions, and their changes throughout the follow-up were based on health interviews.
RESULTS: Based on linear mixed-effect models, midlife physically strenuous work, excess body weight, smoking, cardiovascular disease, hypertension, diabetes mellitus, and asthma predicted muscle strength decline over 22 years of follow-up (P < .05 for all). In addition, pronounced weight loss, becoming physically sedentary, persistent smoking, incident coronary heart disease, other cardiovascular disease, diabetes mellitus, chronic bronchitis, chronic back syndrome, long-lasting cardiovascular disease, hypertension, and asthma were associated with accelerated handgrip strength decline (P < .05 for all).
CONCLUSION: Lifestyle and physical health earlier in life determine rate of muscle strength decline in old age. Efforts should be made to recognize persons at risk in a timely manner and target early interventions to middle-aged persons to slow down muscle strength decline and prevent future functional limitations and disability.
人工透析中の運動療法
あまり質はよくないのですが、人工透析中の運動療法で身体機能が改善するという論文を一応、紹介します。
Gołębiowski T, Kusztal M, Weyde W, Dziubek W, Woźniewski M, Madziarska K, Krajewska M, Letachowicz K, Strempska B, Klinger M. A Program of Physical Rehabilitation during Hemodialysis Sessions Improves the Fitness of Dialysis Patients. Kidney Blood Press Res. 2012 Feb 22;35(4):290-296. [Epub ahead of print]
リサーチクエスチョンは以下の通りです。
P:人工透析を行っているCKD患者29人に
E:透析中にcycle trainingを3ヶ月間行うと、
C:なし
O:身体機能、栄養、炎症が改善するか
Cの比較群がない介入研究ですので、エビデンスレベルはかなり低いです。
結果ですが、6分間歩行テスト、膝の伸展・屈曲の筋力はcycle trainingの前後で有意に改善しました。栄養や炎症には変化がありませんでした。有害事象は観察されませんでした。以上より、人工透析中のcycle trainingは安全で、歩行能力と下肢筋力を有意に改善させるという結論です。
介入研究で有効かどうかを判断するためには、比較群の設定が必要です。比較群を設定しないで、トレーニング前後だけで比較しても、バイアスが大きいので、質の低いエビデンスにしかなりません。そのため、この結論をそのまま鵜呑みにすることはできません。この論文だけでは人工透析中の運動療法を推奨できません。
また、人工透析中の運動療法で栄養状態や炎症が改善しなかったのも残念です。今回の人工透析患者のうち、何人が悪液質に該当するかどうかは不明です。ただ、運動療法による抗炎症作用と栄養改善は今回の研究では見られませんでした。こちらへの関心が高いのでこの論文を読んでみたのですが残念でした。
Abstract
Aim: The aim of the present study was to evaluate the influence of cycle exercise during hemodialysis (HD) on patients' physical proficiency, muscle strength, quality of life and selected laboratory parameters.
Patients and Methods: In a group of 29 (15 female, 14 male) HD patients (age 64.2 ± 13.1 years), 3 months of cycle training during dialysis sessions was performed. The following data were analyzed: strength of lower extremities (six-minute walk test, isokinetic knee extension, flexion peak torque), nutrition parameters (albumin, BMI), inflammation intensity (CRP, IL-6), and quality of life (SF-36v2).
Results: In the six-minute walk test, the increase in walk velocity was 4% (3.56 km/h before and 3.73 km/h after cycle training; p < 0.01). At angular velocity (AV) of 60°/s, extension peak torque in the knee joint rose by 7% and at AV of 300°/s by 4% (p = 0.04). Flexion peak torque at AV of 180°/s increased by 13% (p = 0.0005). The program does not influence nutrition or inflammation parameters. No complications directly related to exercise were observed.
Conclusion: Cycle exercise during dialysis is safe even in older HD patients with multiple comorbidities. It results in a significant increase in general patient walking ability and in a gain in lower extremity muscle strength.
Gołębiowski T, Kusztal M, Weyde W, Dziubek W, Woźniewski M, Madziarska K, Krajewska M, Letachowicz K, Strempska B, Klinger M. A Program of Physical Rehabilitation during Hemodialysis Sessions Improves the Fitness of Dialysis Patients. Kidney Blood Press Res. 2012 Feb 22;35(4):290-296. [Epub ahead of print]
リサーチクエスチョンは以下の通りです。
P:人工透析を行っているCKD患者29人に
E:透析中にcycle trainingを3ヶ月間行うと、
C:なし
O:身体機能、栄養、炎症が改善するか
Cの比較群がない介入研究ですので、エビデンスレベルはかなり低いです。
結果ですが、6分間歩行テスト、膝の伸展・屈曲の筋力はcycle trainingの前後で有意に改善しました。栄養や炎症には変化がありませんでした。有害事象は観察されませんでした。以上より、人工透析中のcycle trainingは安全で、歩行能力と下肢筋力を有意に改善させるという結論です。
介入研究で有効かどうかを判断するためには、比較群の設定が必要です。比較群を設定しないで、トレーニング前後だけで比較しても、バイアスが大きいので、質の低いエビデンスにしかなりません。そのため、この結論をそのまま鵜呑みにすることはできません。この論文だけでは人工透析中の運動療法を推奨できません。
また、人工透析中の運動療法で栄養状態や炎症が改善しなかったのも残念です。今回の人工透析患者のうち、何人が悪液質に該当するかどうかは不明です。ただ、運動療法による抗炎症作用と栄養改善は今回の研究では見られませんでした。こちらへの関心が高いのでこの論文を読んでみたのですが残念でした。
Abstract
Aim: The aim of the present study was to evaluate the influence of cycle exercise during hemodialysis (HD) on patients' physical proficiency, muscle strength, quality of life and selected laboratory parameters.
Patients and Methods: In a group of 29 (15 female, 14 male) HD patients (age 64.2 ± 13.1 years), 3 months of cycle training during dialysis sessions was performed. The following data were analyzed: strength of lower extremities (six-minute walk test, isokinetic knee extension, flexion peak torque), nutrition parameters (albumin, BMI), inflammation intensity (CRP, IL-6), and quality of life (SF-36v2).
Results: In the six-minute walk test, the increase in walk velocity was 4% (3.56 km/h before and 3.73 km/h after cycle training; p < 0.01). At angular velocity (AV) of 60°/s, extension peak torque in the knee joint rose by 7% and at AV of 300°/s by 4% (p = 0.04). Flexion peak torque at AV of 180°/s increased by 13% (p = 0.0005). The program does not influence nutrition or inflammation parameters. No complications directly related to exercise were observed.
Conclusion: Cycle exercise during dialysis is safe even in older HD patients with multiple comorbidities. It results in a significant increase in general patient walking ability and in a gain in lower extremity muscle strength.
2012年3月5日月曜日
病院家庭医を目指して~野望達成への道~のブログ紹介
病院家庭医を目指して~野望達成への道~のブログに、3月3日の日本リハ医学会北海道地方会で講演させていただいた内容がよくまとまっているので、紹介させていただきます。
http://blog.livedoor.jp/gp_ken/archives/6792220.html
悪液質に対する運動療法に懐疑的とあるのは、健全だと思います。
EPCRC悪液質ガイドラインは以下よりダウンロードできます。
http://www.epcrc.org/publication_listfiles.php?id=mWdBCMI5eXVlcNFk7Gnq
In cancer patients, physical training and other physical treatment options are beneficial as a preventive procedure to maintain functional status. The activities and training interventions have to be individualized (overall level of recommendation: strong positive; mean consensus 7.92). However, most research has been done in patients treated with curative intent, and it is not clear to what extent physical training is appropriate in patients with advanced cancer/refractory cachexia.
また、藤本先生の「リハビリテーション栄養と口腔」に関する講演の内容もよくまとまっていますので、紹介させていただきます。
http://blog.livedoor.jp/gp_ken/archives/6792188.html
http://blog.livedoor.jp/gp_ken/archives/6792220.html
悪液質に対する運動療法に懐疑的とあるのは、健全だと思います。
EPCRC悪液質ガイドラインは以下よりダウンロードできます。
http://www.epcrc.org/publication_listfiles.php?id=mWdBCMI5eXVlcNFk7Gnq
In cancer patients, physical training and other physical treatment options are beneficial as a preventive procedure to maintain functional status. The activities and training interventions have to be individualized (overall level of recommendation: strong positive; mean consensus 7.92). However, most research has been done in patients treated with curative intent, and it is not clear to what extent physical training is appropriate in patients with advanced cancer/refractory cachexia.
また、藤本先生の「リハビリテーション栄養と口腔」に関する講演の内容もよくまとまっていますので、紹介させていただきます。
http://blog.livedoor.jp/gp_ken/archives/6792188.html
2012年3月4日日曜日
朝倉病院のブログ紹介
先週の第27回日本静脈経腸栄養学会のNSTフォーラムで、「これからのリハNST~リハビリテーションと栄養療法の質向上のために」という発表をしました。その際、大学病院のNSTと朝倉病院のリハNSTを比較して報告したのですが、その様子が朝倉病院のブログに掲載されています。よかったら見ていただければと思います。
神戸Vol2:
こちらは写真も紹介されています。
http://blog.cabrain.net/CN004824/article/id/58413.html
神戸~(続き)
こちらは発表内容の紹介です。
http://blog.cabrain.net/CN004824/article/id/58439.html
次回のJSPENでは朝倉病院の看護師、管理栄養士、PT、OTにぜひ発表してほしいと思っています。
神戸Vol2:
こちらは写真も紹介されています。
http://blog.cabrain.net/CN004824/article/id/58413.html
神戸~(続き)
こちらは発表内容の紹介です。
http://blog.cabrain.net/CN004824/article/id/58439.html
次回のJSPENでは朝倉病院の看護師、管理栄養士、PT、OTにぜひ発表してほしいと思っています。
登録:
コメント (Atom)